
UN system coordination Task Team
on the Implementation of the UN System Common Position
on drug-related matters
What we have learned over the last ten years:
A summary of knowledge acquired and produced by the
UN system on drug-related matters
March 2019
2
Contents
Foreword .............................................................................................................................. 4
1. Introduction .................................................................................................................. 5
2. Health, including the availability of and access to controlled medicines ...................... 6
2.1 Introduction ................................................................................................................ 6
Drug use among women ................................................................................................................ 8
Access to controlled drugs for medical purposes, particularly for the treatment of pain .............. 9
The right to health .......................................................................................................................... 9
2.2 Prevention of illicit drug use and drug use disorders and promoting healthier
populations at different levels and sectors ...................................................................... 11
2.3. Treatment of drug use disorders, rehabilitation, recovery and social reintegration .. 12
2.4 Minimizing the adverse health consequences of drug use: prevention, treatment and
care of HIV, viral hepatitis, other blood-borne infections and tuberculosis ...................... 16
2.5 Drug use, dependence, injecting, prevention and treatment in prison settings.......... 19
Cost-effectiveness of prevention and treatment and return on investment ................................ 21
Stigma and stigmatizing drug policies affect the effectiveness of drug responses ...................... 22
3. Effective law enforcement and protection of vulnerable communities ..................... 23
3.1 Prevention of drug-related crime .............................................................................. 23
3.2 Response to drug-related crime................................................................................. 24
3.3 Countering trafficking in narcotic drugs and psychotropic substances ....................... 26
3.4 Proportionate and effective policies and responses (including evidence on alternatives
to incarceration and decriminalization/depenalization of drug use) ................................ 28
3.5 Legal guarantees and safeguards pertaining to criminal justice proceedings and the
justice sector (including legal aid and the right to a fair trial) .......................................... 32
3.6 Addressing links between drug trafficking and peace and security (money-laundering,
corruption, armed conflict, and political fragility and stability) ........................................ 32
4. Alternative development ........................................................................................... 35
5. Cross-cutting (or topical) issues .................................................................................. 36
5.1 New psychoactive substances ................................................................................... 36
5.2 Non-medical use of pharmaceuticals ......................................................................... 36
5.3 Use of internet for drug-related activities .................................................................. 37
5.4 Social inclusion .......................................................................................................... 37
5.5 Information (monitoring, epidemiology and statistics) .............................................. 38
6. Treaties and resolutions on international drug policy ................................................ 38
7. Concluding observations ............................................................................................. 42
3
Annex I United Nations system common position supporting the implementation of the
international drug control policy through effective inter-agency collaboration .................. 44
Annex II Summary of key messages based on the knowledge produced and acquired by the
UN system on drug-related matters ................................................................................... 48
Annex III Examples of joint programmes between UN entities on drug-related matters ... 52

4
Foreword
In November 2018, the heads of the UN system came together through the Chief Executives
Board to forge a common position on the question of global drug policy to advance security,
development and human rights. This action was in response to the growing need to provide
multidimensional support to Member States on drug related matters.
Our efforts are rooted in a shared understanding: by integrating analysis and assistance we can
address prevention and treatment, promote alternative development and access to essential
medicines, and enhance justice and law enforcement responses that stop organized crime and
protect people.
To help boost coordination across the system and deliver more effective assistance, we
established a Task Team to produce timely briefs and encourage joint-programming and
resource mobilization for drug-related programmes.
This first such brief is a collection of successful experiences in law enforcement, prevention,
health care, human rights and development over the last ten years. It is a tool for sharing best
practices and promoting evidence-based, rights-based approaches.
I strongly encourage interested parties to support the work of this Task Team. I have no doubt
that, together, we can reduce supply and demand, protect health and human rights, and
contribute to sustainable development, as envisaged in the outcome document of the 2016
United Nations General Assembly Special Session on Drugs.
Let us continue to strengthen our shared commitments and accelerate progress in addressing
the world drug problem in the comprehensive way that our experience proves yields the most
effective results.

5
1.
Introduction
Drug markets are evolving at unprecedented speed. The range of substances and combinations
available to users has never been wider, and the amounts produced have never been greater.
Cultivation and manufacturing of heroin and cocaine have reached record highs, synthetic
drugs continue to expand, and the market for new psychoactive substances (NPS) remains
widely diversified with a growing interplay with traditional drug markets. The non-medical use
of regulated prescription drugs (either diverted from licit channels or illicitly manufactured) is
becoming a major threat: in addition to the ongoing opioid epidemic in North America, there
are signs of an opioid epidemic due to the non-medical use of tramadol in North and sub-
Saharan Africa, as well as in the Middle East. Drug-related deaths are on the rise. At the same
time, access to controlled drugs for medical purposes remains a dramatic problem in most low-
and middle-income countries.
Reasons for blooming drug markets are complex and diversified. A combination of poverty,
limited social and economic opportunities of rural communities, political instability, lack of
government control, and changed strategies of trafficking organizations has driven the high
level of illicit crop cultivation. There remain multiple factors at individual, micro and macro
level that affect the vulnerability to drug use and its path to harmful use. While progress has
been made by some countries to increase the accessibility to human-rights and evidence-
based policy interventions, challenges remain with insufficient investment and implementation
of schemes to prevent, treat and reduce the potential harms posed by drug use. In contrast to
an increasing trend of donors’ commitment for overall international assistance, assistance in
the sectors of alternative development and “narcotics control” has significantly declined since
2008.
1
Punitive drug policies continue to be used in some communities, despite being
ineffective in reducing drug trafficking or in addressing non-medical drug use and supply, and
continue to undermine the human rights and well-being of persons who use drugs, as well as
of their families and communities.
The SDG 2030 Agenda is putting the dignity, health and rights of people and planet at the
centre of sustainable development.
Drug matters are intertwined with all aspects of sustainable development. All areas of the
17 Sustainable Development Goals shape the nature and dynamic of the drug problem. At the
same time, the impact of the drug problem and the response thereto on development can be
observed at individual, community and national levels. For example, ensuring healthy lives and
promoting well-being for all (SDG 3) requires effective measures to address the world drug
problem, while the lucrative drug trade compounds corruption risk and undermines
responsive, accountable and transparent institutions at all levels (SDG 16).
When well-designed drug policy interventions directly or indirectly result in an improvement
in the level of development of their target populations, operations designed to improve
sustainable development can address the vulnerability of people or communities affected by
the drug problem and can ultimately help address it. However, if not based on human rights
standards and a solid evidence base, drug policies can have a counterproductive effect on
1
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).

6
development. Abusive, repressive and disproportionate drug control policies and laws are
counterproductive, while also violating human rights, undercutting public health and wasting
vital public resources.
The outcome document of UNGASS 2016 highlighted the need to strengthen cooperation
among UN entities in their efforts to address the world drug problem, and the need to promote
the protection of and respect for human rights by supporting Member States in the
implementation of the operational recommendations contained in that document. On
7 November 2018, members of the Chief Executives Board for Coordination (CEB) committed
to supporting each other’s activities so as to deliver a “truly balanced, comprehensive,
integrated, evidence-based, human rights-based, development-oriented and sustainable
support to Member States in implementing joint commitments to address the world drug
problem, including the operational recommendations contained in the outcome document of
the 2016 UN General Assembly Special Session on the World Drug Problem”. The CEB also
established a UN system coordination Task Team composed of all interested UN entities and
led by UNODC, for the purposes of coordinating data collection to promote scientific, evidence-
based implementation of international commitments.
2.
Health, including the availability of and access to controlled
medicines
2.1 Introduction
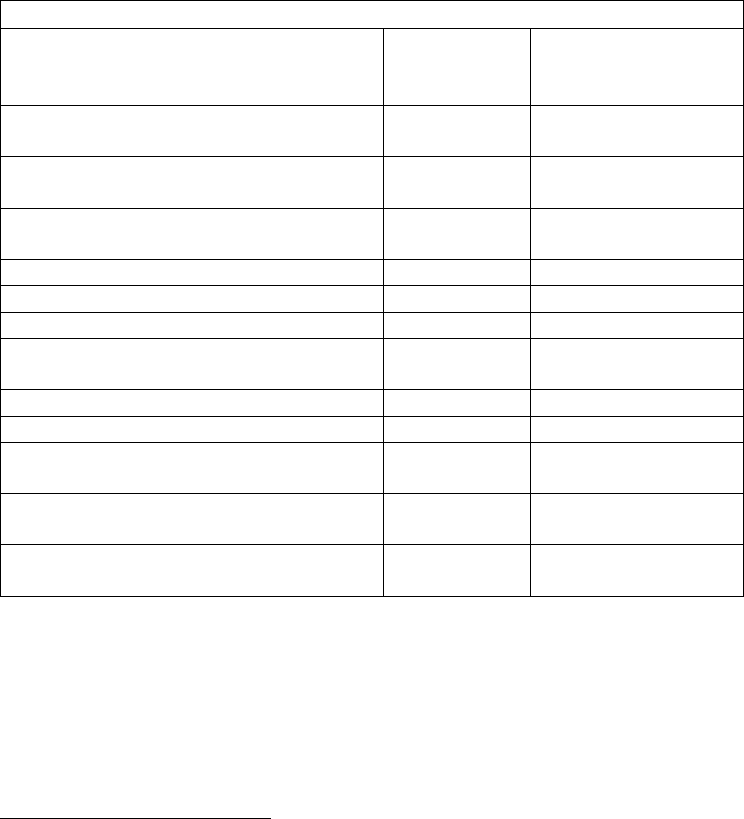
Extent of drug use and overall impact on health
Global extent of drug use in numbers
P
eople
aged 15
–
64 years
who used drugs at
least once in the previous year (2016)
275 million
5.6 per cent
Cannabis 192 million 3.9 per cent
Opioids
Opiates
34.3 million
19.4 million
0.70 per cent
0.40 per cent
Cocaine 18.2 million 0.37 per cent
Amphetamines and prescription
stimulants
34.2 million 0.70 per cent
Ecstasy
20.6 million
0.42 per cent
People aged 15
–
16 years old
who used
cannabis at least once during the previous
year (2016)
13.8 million
5.6 per cent
People aged 15–64 years who suffer from
drug use disorders (2016)
30.5 million 0.62 per cent
People who injected drugs
–
PWID
–
(2016)
10.6 million
0.22 per cent
P
ercentage of people who inject drugs and
their sexual partners among newly infected
people with HIV outside of sub-Saharan
Africa
25 per cent

7
People who injected drugs living with HIV
(2016)
1.3 million 11.8 per cent of PWID
People who injected drugs living with
hepatitis C (2016)
5.5 million 51.9 per cent of PWID
Deaths attributed to the use of drugs (2017)
585,000 72 per cent of deaths
among males
“Healthy” life lost (DALYs) 42 million years 70 per cent of years
of life lost by males
Source: UNODC, World Drug Report 2018; Institute for Health Metrics and Evaluation, Global Burden of Disease
Data; UNAIDS, Global AIDS Update 2018 – Miles to Go (Geneva, 2018); UNAIDS estimates.
Drug use is linked to a range of health, social and protective factors. Thanks to the large body
of scientific literature, there is today a better understanding of what increases an individual’s
vulnerability to initiating the use of substances and what leads to drug use disorders.
2
Lack of
knowledge about substances and their consequences, genetic predisposition, personality traits
(e.g. impulsivity, sensation seeking), the presence of mental health conditions and behavioural
disorders, family neglect and abuse, poor attachment to school and the community, social
norms and environments conducive to substance use (including the influence of media), and
growing up in marginalized, stigmatized and deprived communities are among the main
vulnerability factors. Conversely, psychological and emotional well-being, personal and social
competence, a strong attachment to caring and effective parents, attachment to schools and
communities that are well resourced and organized are all protective factors that contribute
to individuals being less vulnerable to illicit drug use and other risky behaviours.
3
Some of the vulnerability and resilience factors differ according to age. Parenting and
attachment to school are important during infancy, childhood and early adolescence. At older
ages, schools, workplaces, entertainment venues and the media contribute to making
individuals more or less vulnerable to drug use and other risky behaviours.
4
Marginalized youth
in poor communities who have little or no family support, as well as limited access to education
in school, are especially at risk. So are children, individuals and communities torn or displaced
by war or natural disasters.
5
Higher socioeconomic groups have a greater propensity to initiate
illicit drug use than lower socioeconomic groups, but it is the lower socioeconomic groups that
pay the higher price as they are more likely to become drug dependent.
6
Vulnerability factors are largely out of the control of the individual and are linked to a multitude
of social, environmental and health conditions, requiring interventions that address not only
drugs but also other risk factors.
7
The extent of illicit drug use has a negative impact in achieving SDG 3 “Ensure healthy lives and
promote well-being for all at all ages”, not only because of the medical conditions resulting
2
UNODC/WHO, International Standards on Drug Use Prevention, Second updated edition (Vienna, 2018).
3
Ibid.
4
Ibid.
5
Ibid. and UNHCR/WHO, Rapid Assessment of Alcohol and Other Substance Use in Conflict-affected and
Displaced Populations: A Field Guide.
6
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).
7
UNODC/WHO, International Standards on Drug Use Prevention, Second updated edition (Vienna, 2018).

8
directly from the psychoactive and physiological effects of drugs, but also because of the risk
factors associated with certain forms of drugs and modes of administration.
Limited access to services, including health services, and exclusion from relevant host
population programmes, may exacerbate the harmful consequences of illicit drug use and its
negative impact on SDG 3,
8
while also undermining the human rights obligations to address
the HIV epidemic within the community of people who use drugs.
9
Drug use among women
Men are three times more likely than women to use cannabis, cocaine and amphetamines,
whereas women are more likely than men to have a non-medical use of prescription opioids
and tranquillizers. Existing research points to unequal opportunities (also relating to social and
cultural norms) in access to illicit drug markets as one of the reasons for differences in the
prevalence of drug use between men and women. In addition, drug use during pregnancy may
lead to health problems for the pregnant woman and fetus, especially when combined with
alcohol use, malnutrition and low access to health care. Women who use drugs can face
substantial barriers to accessing services, including HIV services – facing lack of accessible
services, stigma and discrimination,
10
in breach of their human rights and undermining the
achievement of SDG 5 “Achieve gender equality and empower all women and girls”.
Service uptake in general and for pregnant women in particular can be improved where there
is support from family members, social connections within the health-care system and referral
services from NGOs
11
and if health workers provide the advice, support, treatment and care in
line with the international guidelines developed for this purpose.
12
Mothers with a history of
drug use often fear accessing health and social services due to stigma and discrimination and
due to legislation that may declare them unfit to parent, while pregnant women may be
pressured to have abortions or to give up newborn infants.
13
There have been reports of
women who use drugs during pregnancy being arrested, confined and forced to undertake
medical treatment, sometimes without evidence that they have drug dependency or that the
health of the fetus is at risk, in clear violation of their rights to freedom from forced treatment,
arbitrary detention and to fair trial.
14
Avoiding stigma and discrimination against women in
health care settings and elsewhere increases their accessibility to services. As WHO has noted,
8
UNHCR/WHO, Rapid Assessment of Alcohol and Other Substance Use in Conflict-affected and Displaced
Populations: A Field Guide.
9
A/65/255.
10
UNODC, World Drug Report 2018 (United Nations publication, Sales No. E.18.XI.9).
11
UNAIDS, The Gap Report (Geneva, 2014).
12
WHO, Guidelines for the identification and management of substance use and substance use disorders in
pregnancy (Geneva, 2014).
13
UNAIDS, Do no harm – health, human rights and people who use drugs (Geneva, 2016).
14
Report of the Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard
of physical and mental health, 3 August 2011, A/66/254, paras. 38, 39; Report of the Working Group on
Arbitrary Detention on its visit to the United States of America, 17 July 2017, A/HRC/36/37/Add.2, paras. 72–74;
Report of the Working Group on Arbitrary Detention on its visit to the United States of America, 17 July 2017,
A/HRC/36/37/Add.2, para. 73.

9
“It is important that all women from key populations have the same support and access to
services related to conception and pregnancy care, as women from other groups.”
15
Access to controlled drugs for medical purposes, particularly for the treatment of pain
The medical use of narcotic drugs continues to be indispensable for the relief of pain and
suffering and ensuring their availability for such purposes is essential. Making internationally
controlled drugs available for medical and scientific purposes is at the heart of the international
drug control conventions since the Single Convention on Narcotic Drugs of 1961. The United
Nations human rights mechanisms also recognized that ensuring access to essential drugs is
an essential element of the right to health.
16
This principle has continued to be emphasized as
the cornerstone of international drug policy in CND resolutions and in the outcome document
of the 2016 UN General Assembly Special Session on the World Drug Problem. Achieving a
balance between ensuring the availability of narcotic drugs and psychotropic substances under
international control for medical and scientific purposes and preventing their diversion and
abuse is at the core of the international drug control system. Both sides of this balance –
ensuring availability and preventing diversion and abuse – are concerned with the protection
and promotion of health and public safety and directly relate to the achievement of SDG 3,
including Target 3.b “Support the research and development of vaccines and medicines …
provide access to affordable essential medicines …”.
Despite international attention, it is clear that there is a large burden of untreated pain around
the world with 80 per cent of the world’s population still without access to controlled
medicines.
17 ,
18
There is a significant divide:
approximately 90 per cent of the morphine
worldwide is consumed by only 17 per cent of the global population living primarily in a few
Western countries.
19,
20
Barriers to accessibility of controlled drugs for medical use include the
limited capacity of health care professionals due to lack of university curricula on the use of
pain medications that are evidence-based, and national policies that may not meet the
regulatory requirements across the full spectrum of the supply chain for controlled essential
medicines.
The right to health
The dignity of human beings, and their right to health, is the cornerstone of effective
international drug policy. Health is a fundamental human right indispensable for the exercise
of other human rights. The enjoyment of the right to health includes, inter alia, access to health
facilities, goods and services that are scientifically and medically appropriate and of good
15
WHO, Consolidated guidelines on HIV prevention, diagnosis, treatment and care for key populations.
16
A/HRC/30/65, para. 33, A/65/255, paras. 40–47, 76.
17
UNODC, Ensuring availability of controlled medications for the relief of pain and preventing diversion and
abuse: Striking the right balance to achieve the optimal public health outcome, Discussion paper based on a
scientific workshop held in Vienna on 18–19 January 2011.
18
UNODC, Technical guidance: Increasing access and availability of controlled medicines, Advanced draft (March
2018).
19
INCB, Special Reports, beginning in 2010.
20
INCB, Special Report: Availability of Internationally Controlled Drugs: Ensuring Adequate Access for Medical
and Scientific Purposes (2015).

10
quality, and the “right to be free from interference, such as the right to be free from torture,
non-consensual medical treatment and experimentation”.
21
The enjoyment of the highest attainable standard of health applies to every human being
without distinction of race, religion, political belief, economic or social condition.
22
The right to
health for all people means that everyone should have access to the health services they need,
when and where they need them, without suffering financial hardship.
23,
24
Yet only one in six
persons with drug use disorders benefits from drug treatment services.
25
Incorporating public health, the reduction of harm from drug use – referred by some
practitioners as harm reduction – and gender-sensitive approaches into national drug
strategies, while ensuring the availability of treatment services that are evidence-based and
respectful of the rights of persons who use drugs, their families and communities, in
accordance with international human rights obligations.
26
Under the right to health and the
right to life, individuals, including children, have a right to services to reduce the harm of non-
medical use of drugs that are accessible, available, acceptable and of good quality.
27,
28
Stigma and discrimination in health care settings can have a significant effect on accessing
services, including HIV testing and treatment. Studies among people who inject drugs found
that respondents were almost seven times as likely to avoid HIV testing if they had been
previously refused treatment or services by health care workers.
29
Negative attitudes of health
care workers towards people with drug use disorders can negatively affect key populations
(KPs).
30
Of the 117 countries reporting to UNAIDS in 2017, only 18 reported that they had anti-
discrimination laws or provisions that apply to people who use drugs (either through health
status or disability).
31
21
CESCR, General comment No. 14 (2000), E/C.12/2000/4, para. 12 (d).
22
UNGA, International Covenant on Economic, Social and Cultural Rights, article 2.2., in conjunction with 16
December 1966, United Nations, Treaty Series, vol. 993, p. 3.
23
Preamble to the Constitution of the WHO. Available at https://www.who.int/governance/eb/who
_constitution_en.pdf.
24
UN General Assembly, International Covenant on Economic, Social and Cultural Rights, article 2.2., in
conjunction with 16 December 1966, United Nations, Treaty Series, vol. 993, p. 3.
25
UNODC, World Drug Report 2018 (United Nations publication, Sales No. E.18.XI.9).
26
See E/C.12/CAN/CO/6, E/C.12/ESP/CO/5, E/C.12/PHL/CO/5-6, E/C.12/GRC/CO/2, E/C.12/MKD/CO/2-4 and
E/C.12/SWE/CO/6.
27
See e.g. CESCR, Concluding Observations on the combined fifth and sixth periodic reports of the Philippines,
E/C.12/PHL/CO/5-6 (2016), para. 54; CESCR, Concluding Observations on the combined second to fourth
periodic reports of the former Yugoslav Republic of Macedonia, E/C.12/MKD/CO/2-4 (2016), para. 52; Report of
the Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard of physical
and mental health, Anand Grover (2010), A/65/255, para. 55.
28
CRC, General comment No. 21 on children in street situations (2017), CR/GC/21 (2017), para .53; CRC,
General comment No. 15 on the right of the child to the highest attainable standard of health (2013),
CRC/C/GC/ 15, para 66.
29
Ti L, Hayashi K, Kaplan K, Suwannanwong P, Wood E, Montaner J et al., “HIV test avoidance among people
who inject drugs in Thailand”, AIDS and Behavior, vol. 17, No. 7 (2013), pp. 2474–2478.
30
Thailand, Ministry of Public Health, International Health Policy Program, Measuring HIV-related Stigma and
Discrimination in Health Care Settings in Thailand: Report of a pilot: Developing Tools and Methods to Measure
HIV-related Stigma and Discrimination in Health Care Settings in Thailand (2014).
31
See http://www.aidsinfoonline.org/ncpi/libraries/aspx/Home.aspx.

11
The criminalization of drug use for other purposes than medical and scientific ones can have a
negative effect on the enjoyment of the right to health. It can increase stigma and
discrimination and thus deter affected persons from seeking treatment and rehabilitation
services, thereby rendering them more vulnerable to violence and abuse from both private
and state agencies.
Stigma created or reinforced through punitive enforcement or treatment regimes may also
increase health risks. Policing practices ranging from surveillance to use of excessive force have
been noted to target vulnerable and marginalized populations, which may increase the risks of
physical and mental health issues for people who use drugs. It can lead to higher rates of risky
injection practices and can increase risks of overdose due to lack of access to clean syringes or
safe injecting rooms, the need to inject quickly and in unsafe places, and being driven from
areas where services to minimize the harm of drug use are provided, all of which can increase
exposure to HIV and other blood borne infections.
32
2.2 Prevention of illicit drug use and drug use disorders and promoting healthier
populations at different levels and sectors
Substance use most commonly begins in adolescence, with alcohol, tobacco and cannabis
being the substances most commonly used by children and young people. Early onset of
frequent substance use is associated with the increased risk of developing dependence or
harmful use later in life, as well as being linked with physical and mental health problems,
although there is no clear causal relationship. Effective prevention starts early and is based on
the best available scientific evidence. Many sectors have a role to play, primarily the health
sector, but the education sector can also play a key role in protecting children and young
people from substance use,
33
and at the same time can promote an environment where
seeking treatment for problematic drug use is not stigmatized.
SDG Target 3.5 “Strengthen the prevention and treatment of substance abuse, including
narcotic drug abuse and harmful use of alcohol” defines the importance of providing
prevention and treatment services in the context of sustainable development. The second
updated edition of the UNODC and WHO International Standards on Drug Use Prevention
34
summarizes the currently available scientific evidence on interventions and policies that have
been found to be effective in preventing drug use, as well as other related risky behaviours.
Effective interventions and policies have been identified across many settings (family, school,
community, workplace, health sector, etc.) and levels of risk (universal, selective and
indicated).
35
In infancy and early childhood, effective actions are: prenatal and infancy
visitation, interventions targeting pregnant women, and early childhood education. For middle
childhood (approximately 5 to 10 years of age), effective strategies include: parenting skills
programmes (effective also in early adolescence), personal and social skills education,
classroom environment improvement programmes, policies to retain children in school, as well
32
A/65/255 paragraph 24.
33
UNESCO/UNODC/WHO, Education sector responses to the use of alcohol, tobacco and drugs (Paris, 2017).
34
See https://www.unodc.org/unodc/en/prevention/prevention-standards.html.
35
Ibid.

12
as addressing mental health disorders (relevant also in adolescence). In early adolescence,
additional effective strategies include: prevention education based on social competence and
influence, school policies on substance use, school-wide programmes to enhance school
attachment, addressing individual psychological vulnerabilities, and mentoring. In later
adolescence and adulthood, additional effective strategies include: brief intervention, tobacco
and alcohol policies, as well as multi-component programmes in the workplace, in the
community and in entertainment venues. Media campaigns can also play an important
supportive role
36
without stigmatizing people who use drugs.
There is limited research on the different factors that may influence a different efficiency of
prevention programmes for males and females. The little available evidence points to some
different etiological factors for women and girls.
37
Commercial determinants of health in the case of legally produced and distributed substances
such as dependence-producing prescription drugs can also influence the scope and nature of
drug use. The rapidly growing cannabis industry has become a new part of the private
commercial sector in some countries that can promote cannabis products and choices that
could be detrimental to health. These conditions are additional elements that can make
prevention activities and policies more or less effective.
Health professionals are in a unique position to identify psychoactive substance use among
their clients and intervene at an early stage before substance use disorders and serious related
problems develop. There is substantial accumulated evidence of the effectiveness of screening
and brief interventions for hazardous and harmful alcohol use in primary health care settings.
38
Research findings suggest that screening followed by brief interventions can also be effective
when targeting drugs other than alcohol psychoactive substances. The WHO ASSIST package
helps health professionals to intervene at early stages of substance use to prevent
development of substance use disorders.
39
2.3. Treatment of drug use disorders, rehabilitation, recovery and social reintegration
Drug use dependence is a complex, multifactorial health disorder characterized by a chronic
and relapsing nature that requires a multidisciplinary and comprehensive response, including
diversified pharmacological and psychosocial interventions.
40,
41
The main treatment recommended by WHO for opioid use disorders is opioid substitution
therapy (OST) with long acting opioids (methadone and buprenorphine, both of which are on
the WHO List of Essential Medicines).
42
OST (also called opioid agonist maintenance
36
Ibid.
37
UNODC, Guidelines on drug prevention and treatment for girls and women (Vienna, 2016).
38
Kaner EFS et al. (2018).
39
WHO, mhGAP Intervention Guide for mental, neurological and substance use disorders in non-specialized
health settings, Version 2.0 (2016).
40
UNODC, World Drug Report 2015 (United Nations publication, Sales No. E.15.XI.6).
41
UNODC, Outcome document of the 2016 United Nations General Assembly Special Session on the World Drug
Problem: Our joint commitment to effectively addressing and countering the world drug problem (2016).
42
WHO, Guidelines for the psychosocially assisted pharmacological treatment of opioid dependence (2009).

13
treatment), combined with psychosocial assistance, has been found to be the most
effective.
43
Another option is detoxification followed by relapse-prevention treatment using
opioid antagonist (naltrexone).
44
Psychosocial interventions are the treatment options available for drugs other than opioid.
45
There is no medication proven effective for managing and treating stimulant use disorders.
46
With regard to psychosocial interventions, the evidence from clinical trials supports the
effectiveness of cognitive behavioural therapy (CBT), motivational interviewing (MI),
community reinforcement approach (CRA), motivational enhancement therapy (MET), family
therapy (FT), contingency management (CM) and 12-step group facilitation.
47
Health care systems oftentimes struggle to appropriately respond to behavioural and medical
problems caused by different types of drugs. For example, in parts of the world where opioids
were seldom used, health systems do not have the capacity to deliver medically assisted
treatment, such as opioid agonist maintenance therapy. Similarly, where the treatment system
has mainly focused on opioid use disorders, the system is challenged to respond to an increase
in psychostimulants use disorders for which evidence-based psychosocial treatment is the
main effective intervention in the absence of evidence-based pharmacological treatment.
As mentioned above, criminalization of drug use and law enforcement practices can act as a
barrier to accessing treatment, as can concerns of confidentiality, particularly where drug
registers are utilized. Stigma and discrimination by health care professionals similarly can limit
willingness to engage in drug dependence treatment.
48
Opioid overdose is manageable with naloxone, an opioid antagonist that rapidly reverses the
effects of opioids. Naloxone can be injected intramuscularly, subcutaneously, intravenously or
administered intranasally. According to WHO guidelines, community distribution of naloxone
will reduce overdose deaths.
49
Management of opioid overdose with naloxone is expected to
reduce opioid overdoses that result in death. An overall prevention strategy would also include
access to effective treatment of opioid use disorders.
50
Heroin-assisted treatment refers to the prescription of synthetic, injectable or smokable heroin
to a minority of people with opioid dependence who do not respond to treatment with one of
the established medications used in long-acting agonist maintenance therapy, such as
43
Ibid.
44
Ibid.
45
UNODC/WHO, Principles of Drug Dependence Treatment (2008); UNODC/WHO, International Standards for
the Treatment of Drug Use Disorders: Draft for Field Testing (2016).
46
Ibid.
47
mhGAP Evidence Resource Centre on drug use disorders; UNODC/WHO, Principles of Drug Dependence
Treatment (2008); UNODC/WHO, International Standards for the Treatment of Drug Use Disorders: Draft for
Field Testing (2016).
48
Report of the Special Rapporteur on the right of everyone to the enjoyment of the highest attainable standard
of physical and mental health, Anand Grover (2010), A/65/255, paras. 30–39.
49
WHO 2014.
50
UNODC/WHO, Opioid Overdose: Preventing and Reducing Opioid Overdose Mortality (2013); WHO,
Community management of opioid overdose (2014).

14
methadone or buprenorphine. For this small group of patients, heroin-assisted treatment has
been found effective in improving their social and health situation. It has also been shown to
be cost-effective, as it reduces costs of arrests, trials, incarceration and health interventions.
In this approach, patients are provided with a form of pharmaceutical-grade heroin (injection)
solution.
The public health system is best placed to take the lead in the provision of effective treatment
services for people affected by drug use disorders, often in close coordination with social care
services and other community services.
51
The public health approach to drug treatment
involves the least invasive intervention possible with the highest level of effectiveness and the
lowest cost possible.
52
The right to health includes “the right to be free from … non-consensual medical treatment
and experimentation.”
53
WHO and UNODC have stated, “The same standards of ethical
treatment should apply to the treatment of drug dependence as other health care conditions.
These include the right to autonomy, and self-determination on the part of the patient, and
the obligation for beneficence and non-maleficence [do good/do no harm] on behalf of
treating staff.”
54
Neither detention nor forced labour is based on evidence of effectiveness and
they have no therapeutic value as treatment for drug use disorders.
55
People who use or are
dependent on drugs do not automatically lack the capacity to consent to treatment. Therefore,
treatment should not be forced or against the will and autonomy of the patient and the
consent of the patient should be obtained before any treatment intervention. In 2012, 12 UN
entities raised concerns about drug detention centres and rehabilitation centres as places that
raise human rights issues and threaten the health of detainees and called for their immediate
closure, for an end to financial and technical support for such centres and for investigations to
address abuses.
56
Incarceration and confinement in compulsory drug treatment centres often
worsens the lives of drug users and drug dependent individuals, particularly the youngest and
most vulnerable.
57
According to the Special Rapporteurs, compulsory drug treatment centres
also breach the rights to freedom from arbitrary detention and can amount to torture and
inhuman and degrading treatment or punishment.
58
51
UNODC/WHO, Principles of Drug Dependence Treatment (2008); UNODC/WHO, International Standards for
the Treatment of Drug Use Disorders: Draft for Field Testing (2016).
52
Ibid.
53
CESCR, General comment No. 14 on the right to the highest attainable standard of health, E/C.12/2000/4,
adopted 11 August 2000, para. 34; see also CESCR, General comment No. 14 on the right to the highest
attainable standard of health, E/C.12/2000/4, adopted 11 August 2000, para. 34; Report of the Special
Rapporteur on the right of everyone to the enjoyment of the highest attainable standard of physical and mental
health (2010), A/64/272; Report of the Special Rapporteur on the rights of persons with disabilities (2018),
A/73/161, paras. 9, 14–15; see also UNODC/WHO, Principles of Drug Dependence Treatment (2008) p. 9.
54
UNODC/WHO, Principles of Drug Dependence Treatment (2008).
55
Ibid.
56
ILO/OHCHR/UNDP/UNESCO/UNFPA/UNHCR/UNICEF/UNODC/UN Women/WFP/WHO/UNAIDS, Joint
Statement: Compulsory drug detention and rehabilitation centres. Available at http://www.unodc.org/
documents/southeastasiaandpacific//2012/03/drug-detention-centre/JC2310_Joint_Statement6March12FINAL
_En.pdf.
57
Jurgens and Betteridge (2005).
58
Report of the Special Rapporteur on torture and other cruel, inhuman or degrading treatment or punishment,
Manfred Nowak (2013), A/HRC/22/53, paras. 42, 87(a); Report of the Special Rapporteur on the right of

15
Drug use or drug dependence alone is not sufficient grounds for detention.
59
Where drug
dependence is considered a disability, the Convention on the Rights of Persons with Disabilities
provides further protection, stating clearly that “the existence of a disability shall in no case
justify a deprivation of liberty.”
60
Compulsory detention, even if it has a basis in law, may also
constitute arbitrary detention where it is random, capricious or disproportionate – that is, not
reasonable or necessary in the circumstances of a given case.
61
Compulsory treatment for
people dependent on drugs can only be legally justified in clearly defined exceptional
circumstances in conformity with international human rights law that guarantees such
provisions are not subject to abuse.
62
The treatment must be scientifically and medically
appropriate and of good quality
63
and intended to return a person to a state of autonomy over
their treatment decisions. It must be short term and specifically time bound.
64
On several occasions, UN human rights bodies have expressed concerns about reports of poor
conditions in drug rehabilitation centres and ill-treatment inflicted upon persons admitted to
them.
65
A number of social and structural barriers continue to hinder the access of women to
treatment for drug use: globally, only one of five drug users in treatment is a woman even
though one of three drug users is a woman.
66
As with men, effective treatment for women
balances individual needs with their drug use disorder and the cultural, structural, ethnic and
everyone to the enjoyment of the highest attainable standard of physical and mental health, Anand Grover
(2010), A/65/255, paras. 30–39.
59
OHCHR, Report of the Working Group on Arbitrary Detention (2015), A/HRC/30/36, para. 60: “Drug
consumption or dependence is not sufficient justification for detention. Involuntary confinement of those who
use or are suspected of using drugs should be avoided.”; Report of the Special Rapporteur on torture and other
cruel, inhuman or degrading treatment or punishment, Juan Mendéz (2013), A/HRC/22/53, paras. 40–42; see
also Report of the Working Group on Arbitrary Detention (2003), E/CN.4/2004/3, paras. 74, 87; Human Rights
Committee, General comment No. 35: Article 9 (Liberty and security of person) (2014), CCPR/C/GC/35, para. 15;
European Court of Human Rights, Witold Litwa v. Poland, Application No. 26629/95, 4 April 2000, paras. 77–80.
60
CRPD, art 14(1)(b).
61
Human Rights Committee, General comment No. 35: Article 9 (Liberty and security of person), CCPR/C/GC/35,
para. 12: “An arrest or detention may be authorized by domestic law and nonetheless be arbitrary. The notion
of ‘arbitrariness’ is not to be equated with ‘against the law’ but must be interpreted more broadly to include
elements of inappropriateness, injustice, lack of predictability and due process of law, as well as elements of
reasonableness, necessity and proportionality. For example, remand in custody on criminal charges must be
reasonable and necessary in all the circumstances. Aside from judicially imposed sentences for a fixed period of
time, the decision to keep a person in any form of detention is arbitrary if it is not subject to periodic re-
evaluation of the justification for continuing the detention.”
62
ILO/OHCHR/UNDP/UNESCO/UNFPA/UNHCR/UNICEF/UNODC/UN Women/WFP/WHO/UNAIDS, Joint
Statement: Compulsory drug detention and rehabilitation centres.
63
In accordance with the right to health, see General comment No. 14 on the right to health, para. 12(d).
64
Human Rights Committee, General comment No. 35: Article 9 (Liberty and security of person), CCPR/C/GC/35,
para 12: “Aside from judicially imposed sentences for a fixed period of time, the decision to keep a person in any
form of detention is arbitrary if it is not subject to periodic re-evaluation of the justification for continuing the
detention.”
65
See e.g. CAT/C/GTM/CO/5-6; CAT/C/TKM/CO/2; CRC/C/PAK/CO/5; CCPR/C/KHM/CO/2; CRC/C/KHM/CO/2; UN
Working Group on Arbitrary Detention Report, A7HRC730-36 (2015), p. 17.
66
UNODC, World Drug Report 2015 (United Nations publication, Sales No. E.15.XI.6).

16
religious factors that may limit their access to evidence-based drug treatment.
67
While data
are limited, there is some evidence that other sub-population groups such as displaced persons
or refugees are disadvantaged in accessing drug treatment.
68
Lesbian, gay, bisexual, transgender and intersex persons who use drugs are disproportionately
impacted by drug policies in many countries and experience a range of harms flowing from
drug use and drug-induced mental trauma. Lesbian, gay, bisexual, transgender and intersex
persons who use drugs may not seek support or treatment from health-care providers because
of previous or anticipated experiences of discrimination.
69
2.4 Minimizing the adverse health consequences of drug use: prevention, treatment
and care of HIV, viral hepatitis, other blood-borne infections and tuberculosis
In some countries where transmission of HIV and viral hepatitis is concentrated in people who
inject drugs, the coverage of evidence-based services remains low or non-existent. WHO has
defined a package of evidence-based prevention, diagnosis and treatment services for HIV and
hepatitis that include needle and syringe programmes, opioid substitution therapy and
community distribution of naloxone, as well as testing and treatment of HIV, viral hepatitis B
and C and TB.
The current low coverage of this package is insufficient to effectively prevent transmission and
ultimately achieve SDG 3.3 “By 2030, end the epidemics of AIDS, tuberculosis, malaria and
neglected tropical diseases and combat hepatitis, water-borne diseases and other
communicable diseases”. Globally, needle and syringe programmes distributed just 33 needles
and syringes per person who injects drugs per year (instead of recommended 200 for HIV and
300 for reaching the WHO HCV elimination targets), and only 16 per cent of people who inject
drugs had access to opioid substitution therapy (instead of the recommended 40 per cent).
Overall, it is estimated that less than 1 per cent of people who inject drugs live in countries
where the coverage of these key interventions is sufficient.
70
People who inject drugs are at 23
times greater risk of HIV infection than people who do not inject drugs,
71
and incidence is not
declining. More than 80 per cent of people who inject drugs are either living with, or have
previously had, a hepatitis C infection.
72
The comprehensive package to effectively prevent HIV includes the nine interventions
described by WHO, UNODC and UNAIDS. The three organizations recommend the provision of
a comprehensive set of evidence-based services to people who inject drugs. The effectiveness
67
UNODC, Guidelines on drug prevention and treatment for girls and women (Vienna, 2016); WHO, Guidelines
for identification and management of substance use and substance use disorders in pregnancy (2014).
68
UNHCR/WHO, Rapid Assessment of Alcohol and Other Substance Use in Conflict-affected and Displaced
Populations: A Field Guide.
69
A/HRC/39/39, para. 75.
70
Sarah Larney and others, “Global, regional, and country-level coverage of interventions to prevent and
manage HIV and hepatitis C among people who inject drugs: A systematic review”, The Lancet Global Health,
vol. 5, No. 12, pp. e1208–e1220.
71
UNAIDS Fact Sheet – World AIDS Day 2018. Available at: www.unaids.org/sites/default/files/media_asset/
UNAIDS_FactSheet_en.pdf.
72
WHO, Global Hepatitis Report 2017 (Geneva, 2017).

17
of a core package of nine services was confirmed in 2009 by the three organizations. In 2014,
WHO updated the package to include opioid overdose management with naloxone for people
who inject drugs and pre-exposure prophylaxis as prevention intervention, alongside
interventions to minimize the adverse health consequences of drug use.
73
In addition to the
health interventions, WHO positioned addressing structural barriers with enabling
interventions as part of a public health response to HIV for key populations including people
who inject drugs. Enabling interventions includes reviewing laws and legislation that
criminalize behaviours such as drug use and possession for personal use, reducing stigma and
discrimination, including in the health sector, and addressing violence, as well as supporting
the empowerment of people who use drugs. Their implementation requires a scale-up through
multiple service delivery models, including outreach, low-threshold drop-in centres and peer
education. These programmes effectively reduce the sharing of injecting equipment, improve
quality of life, decrease mortality, reduce crime and public disorder, improve social functioning
and provide a bridge to drug dependence treatment.
The greatest benefit from HIV and hepatitis C prevention is reported when needle and syringe
programmes are offered in combination with opioid substitution therapy and their coverage is
high,
74,
75,
76
meaning more than 300 needles or syringes per person who injects drugs per year,
and more than 40 per cent of people who inject drugs undergoing opioid substitution
therapy.
77
There is strong evidence that high coverage of needle-syringe programmes and opioid
substitution therapy services — closely linked to condom programming, testing and treatment
of HIV and viral hepatitis — can have a major public health impact in places with substantial
populations of people who inject drugs.
78
Opioid substitution therapy has been found to
73
WHO/UNODC/UNAIDS, Technical guide for countries to set targets for universal access to HIV prevention,
treatment and care for injecting drug users, (Geneva, 2012); WHO, Consolidated guidelines on HIV prevention,
diagnosis, treatment and care for key populations, 2016 update (Geneva, 2016).
74
Louisa Degenhardt and others, “Prevention of HIV infection for people who inject drugs: Why individual,
structural and combination approaches are needed”, The Lancet, vol. 376, No. 9737 (2010), pp. 285–301.
75
Natasha K. Martin and others, “Combination interventions to prevent HCV transmission among people who
inject drugs: Modelling the impact of antiviral treatment, needle and syringe programs, and opiate substitution
therapy”, Clinical Infectious Diseases, vol. 57,
supplement 2 (2013),
pp.
S39–S45.
76
Katy Turner and others, “The impact of needle and syringe provision and opiate substitution therapy on the
incidence of hepatitis C virus in injecting drug users: Pooling of UK evidence” Addiction, vol. 106, No. 11 (2011),
pp.
1978–1988.
77
WHO/UNODC/UNAIDS, Technical guide for countries to set targets for universal access to HIV prevention,
treatment and care for injecting drug users, (Geneva, 2009)
78
Abdul-Quader AS, Feelemyer J, Modi S, Stein ES, Briceno A, Semaan S et al., “Effectiveness of structural-level
needle/syringe programs to reduce HCV and HIV infection among people who inject drugs: A systematic
review”, AIDS and Behavior, vol. 17, No. 9 (2013), pp. 2878–2892.
Waal H, Clausen T, Gjersing L, Gossop M., “Open drug scenes: responses of five European cities”, BMC Public
Health, vol. 14 (2014), p. 853.
Jones L, Pickering L, Sumnall H, McVeigh J, Bellis A, “A review of the effectiveness and cost-effectiveness of
needle and syringe programs for injecting drug users”, Centre for Public Health, Liverpool John Moores
University (2008).
Palmateer N, Kimber J, Hickman M, Hutchinson S, Rhodes T, Goldberg D, “Evidence for the effectiveness of
sterile injecting equipment provision in preventing hepatitis C and human immunodeficiency virus transmission
among injecting drug users: A review of reviews”, Addiction, vol. 105, No. 5 (2010), pp. 844–859.

18
improve access and adherence to antiretroviral therapy, reduce instances of overdose and
associated mortality, and lessen criminal activity.
79
Opioid-substitution therapy (OST), needle-
syringe programmes (NSP) and antiretroviral therapy (ART) together have established
effectiveness in reducing drug dependency, reducing sharing of injecting equipment,
improving quality of life and averting HIV infections.
80
The burden of disease of viral hepatitis attributable to injecting drug use is even higher than
HIV. Of the 71 million people with chronic HCV, 8 per cent is among people who inject drugs.
However, 23 per cent of new HCV infections and 33 per cent of HCV related mortality are
attributable to injecting drug use. The WHO recommendations and elimination targets put a
strong focus on providing these services as well as prioritizing PWID to test and treat for HCV.
HCV is curable and countries that have implemented targeted programmes are likely to reach
the elimination targets.
81
The concern of HIV transmission is not only with people who inject drugs such as opioids. There
is evidence that among people who inject stimulants (cocaine and amphetamines) and among
men who have sex with men, those who use methamphetamine or amphetamine are more
likely to engage in higher-risk sexual behaviours and be HIV-positive than those who use other
drugs.
82
A systematic review found that the risk of acquiring HIV was 3.6 times greater among
people who used cocaine by injection than among those who used cocaine by other means,
and 3.0 times higher among people who used amphetamine-type stimulants by injection than
among those who used amphetamine-type stimulants by other means. Most evidence points
towards a positive
association between stimulant use, higher-risk sexual and injecting
behaviours and HIV infections.
83,
84
Wodak A, Cooney A, “Effectiveness of sterile needle and syringe programs”, International Journal of Drug Policy,
vol. 16, No. 1 (2005), pp. 31–44.
MacArthur GJ, Minozzi S, Martin N, Vickerman P, Deren S, Bruneau J et al., “Opiate substitution treatment and
HIV transmission in people who inject drugs: Systematic review and meta-analysis”, British Medical Journal, vol.
345 (2012), p. e5945.
Degenhardt L, Mathers B, Vickerman P, Rhodes T, Latkin C, Hickman M, “Prevention of HIV infection for people
who inject drugs: Why individual, structural, and combination approaches are needed”, The Lancet, vol. 376,
No. 9737 (2010), pp. 285–301.
Gowing L, Farrell M, Bornemann R, Sullivan L, Ali R, “Substitution treatment of injecting opioid users for
prevention of HIV infection”, Cochrane Database of Systematic Reviews, vol. 2, No. CD004145 (2008).
79
Lawrinson P, Ali R, Buavirat A, Chiamwongpaet S, Dvoryak S, Habrat B et al., “Key findings from the WHO
collaborative study on substitution therapy for opioid dependence and HIV/AIDS”, Addiction, vol. 103, No. 9
(2008), pp. 1484–1492.
80
Degenhardt L et al., “HIV prevention for people who inject drugs: why individual, structural, and combination
approaches are required”, The Lancet, vol. 376, No. 9737 (2010), pp. 285–301; WHO/ UNODC/UNAIDS,
Technical guide for countries to set targets for universal access to HIV prevention, treatment and care for
injecting drug users, 2012 revision (Geneva, 2012).
81
WHO, Global Health Sector Strategy on Viral Hepatitis 2016–2121: Towards Ending Viral Hepatitis (2016);
WHO, Global Hepatitis Report 2017 (Geneva, 2017).
82
Nga Thi Thu Vu, Lisa Maher, and Iryna Zablotska, “Amphetamine-type stimulants and HIV infection among
men who have sex with men: Implications on HIV research and prevention from a systematic review and meta-
analysis”, Journal of the International AIDS Society, vol. 18, No. 1 (2015).
83
Isabel Tavitian-Exley and others, “Influence of different drugs on HIV risk in people who inject: Systematic
review and meta-analysis”, Addiction, vol. 110, No. 4, pp. 572–584.
84
Louisa Degenhardt and others, “Meth/amphetamine use and associated HIV: Implications for global policy
and public health”, International Journal of Drug Policy, vol. 21, No. 5 (2010), pp. 347–358.
19
Women who inject drugs are often more vulnerable to HIV than their male counterparts. A
review of studies in countries with a high prevalence of HIV among people who inject drugs
(greater than 20 per cent) found a higher overall prevalence of HIV among women who inject
drugs compared with men who inject drugs.
85
Unsafe injecting practices may be more common
among women because of the lack of services tailored to their needs.
In many countries, punitive drug policies do not recognize the unique vulnerability of persons
with psychosocial disabilities who use drugs. Such policies affect them negatively by not
providing appropriate drug dependence treatment and services to prevent the adverse health
consequences of drug use.
86
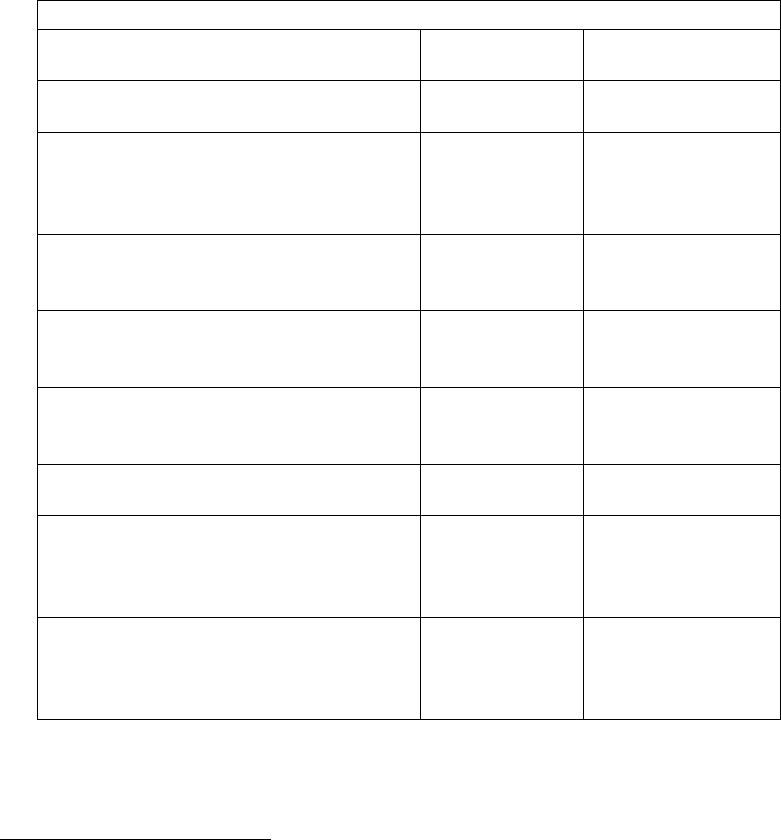
2.5 Drug use, dependence, injecting, prevention and treatment in prison settings
Drug use in prison settings: the numbers
Global prison population (2017)
90 per cent male
1 per cent children
10.7 million 142 people per
100,000 population
Prisoners have used a controlled substance
at some point while incarcerated
33 per cent of
prisoners
Prisoners who have reported current
(past month) drug use
16 per cent of
prisoners
Lifetime prevalence of injection drug use
within prison
Asia
-
Pacific
20.2 per cent
Eastern Europe and Central Asia 17.3 per cent
Latin America and the Caribbean 11.3 per cent
Western and Central Europe and
North America
9.3 per cent
Middle East and North Africa 7.3 per cent
Other African regions less than 1 per cent
People held in prisons who are living
with HIV
3.8 per cent
People held in prisons who are living
with hepatitis C
15.1 per cent
People held in prisons who have active
tuberculosis
2.8 per cent
Source: United Nations Survey on Crime Trends and Operations of Criminal Justice Systems (various years); Note
by the Secretariat: World crime trends and emerging issues and responses in the field of crime prevention and
criminal justice, E/CN.15/2014/5; UNODC, World Drug Report 2017; Babak Moazen and others, “Prevalence of
drug injection, sexual activity, tattooing, and piercing among prison inmates”, Epidemiologic Reviews, vol. 40,
No. 1, (2018), pp. 58–69; Kate Dolan and others, “Global burden of HIV, viral hepatitis, and tuberculosis in
prisoners and detainees”, The Lancet, vol. 388, No. 10049 (2016), pp. 1089–1102.
85
Don C. Des Jarlais and others, “Are females who inject drugs at higher risk for HIV infection than males who
inject drugs: An international systematic review of high seroprevalence areas”, Drug and Alcohol Dependence,
vol. 124, Nos. 1 and 2 (2012), pp. 95–107.
86
A/HRC/39/39, para. 74.

20
Drug-related data on prison populations are limited due to the lack of systematic monitoring
in many countries. Based on global reviews of available national and subnational studies, it is
clear that, in many countries and regions, prison settings are likely to be a place with high drug
use and high-risk injecting practices. But despite this high risk, in some countries, health care
services provided in prisons are not equivalent to those available in the community. This
undermines the overarching principle of the implementation of the SDG of not leaving anyone
behind.
A global systematic review of the literature and national surveys of 189 countries indicated
that 11 countries provided prison-based NSP. Data also indicated that prison-based OST
operated in 56 countries. The study indicated HIV testing and treatment were provided in 79
and 88 countries, respectively.
87
People deprived of their liberty (whether in criminal or administrative detention) have a right
to access health care services, including drug dependence treatment, and services to reduce
the harm of drug use equivalent to those outside prison. According to the Special Rapporteur
on torture and other cruel, inhuman or degrading treatment or punishment, for example, the
denial of methadone treatment in custodial settings has been considered to be a violation of
the right to be free from torture and ill-treatment in certain circumstances.
88
The period shortly after release from prison is associated with a substantially increased risk of
drug-related death (primarily fatal overdose). Drug-related mortality rate after release from
prison has been found to be 50–100 times higher than the mortality rate of the general
population.
89,
90
Women in prison often come from socially marginalized groups and compared with women in
the wider community, they are more likely to have engaged in sex work and/or illicit drug use
and be living with HIV owing to the combined risks of unsafe injecting practices and
unprotected sex.
91, 92
The nine interventions described in the WHO, UNODC, UNAIDS Technical guide for countries
to set targets for universal access to HIV prevention, treatment and care for injecting drug users
93
are appropriate for implementation in prisons and other closed settings. UNODC, ILO, UNDP,
WHO and UNAIDS
94
have defined a specific comprehensive package of interventions for HIV
87
Rebecca Bosworth, Babak Moazen, and Kate Dolan, “HIV, viral hepatitis and TB in prison populations: A global
systematic review and survey of infections and mortality, and provision of HIV services in prisons”
(forthcoming).
88
A/HRC/10/44 and Corr.1, para. 57.
89
WHO, Preventing Overdose Deaths in the Criminal Justice System (Copenhagen, 2014).
90
Elizabeth L. C. Merrall and others, “Meta-analysis of drug-related deaths soon after release from prison”,
Addiction, vol. 105, No. 9 (2010), pp. 1545–1554.
91
UNODC, World Drug Report 2015 (United Nations publication, Sales No. E.15.XI.6).
92
Steffanie Strathdee and others, “Substance use and HIV among female sex workers and female prisoners: Risk
environments and implications for prevention, treatment, and policies”, Journal of Acquired Immune Deficiency
Syndrome, vol. 69, supplement 2, pp. S110–S117.
93
See http://www.unodc.org/documents/hiv-aids/publications/People_who_use_drugs/Target_setting
_guide2012_eng.pdf.
94
See http://www.unodc.org/documents/hiv-aids/HIV_comprehensive_package_prison_2013_eBook.pdf.

21
prevention, treatment and care in prisons and other closed settings. This package of 15
interventions includes all the nine interventions targeting PWID as well as additional
interventions to address broader HIV risk, including interventions for the prevention of
mother-to-child transmission of HIV; measures to combat sexual violence; post-exposure
prophylaxis; precautions to prevent transmission through medical and dental services;
measures to make tattooing, piercing and other forms of skin penetration safer; and
interventions for staff.
95
In general, exposure to the prison environment facilitates affiliation with older criminals and
criminal gangs and organizations. It also increases stigma and helps to form a criminal identity.
It often increases social exclusion, worsens health conditions and reduces social skills.
Alternatives to incarceration within the community (outpatient or residential therapeutic
setting), such as psychosocially supported pharmacological treatment for opiate dependence,
can be more effective than imprisonment in reducing reoffending.
96
Cost-effectiveness of prevention and treatment and return on investment
Investing in prevention and control of drug use and drug use disorders produce significant
returns: saved lives, prevented disabilities, healthier populations, improved workforce
participation and productivity, and reduced criminal justice costs. Every single US$ invested in
effective treatment of substance use disorders can return to societies between $4 and $12.
97
It has been estimated that expenditure on drug treatment produces savings not only for the
health system but also for the criminal justice system.
Services aimed at reducing the harm caused by non-medical drug use are also cost effective.
For example, each dollar spent in a needle-syringe programme can return up to $5.50 in
averted health-care costs. By comparison, incarceration appears expensive and ineffective.
The unit costs of interventions which minimize the adverse health consequences of drug use
are relatively low, but can vary by provider type, delivery model and region. Generally, NSP are
least expensive, while the costs of ART are expected to decline by 2020. OST is a structural
intervention with other societal benefits: when such benefits are included, the attributable
cost for HIV budgets and cost effectiveness ratios are highly favourable. In one particular
country, the expansion of needle-syringe programmes and methadone maintenance therapy
has seen the proportion of HIV infections acquired through injecting drug use plummet from
nearly 50 per cent to less than 1 in 10.
98
Although the overall costs of scaling up programmes to minimize the adverse health
consequences of drug use will be high, it will be a worthwhile action; not only do the societal
benefits of programmes to minimize the adverse health consequences of drug use exceed their
treatment costs, but they also have the potential to provide significant returns on investment
95
WHO, Consolidated guidelines on HIV prevention, diagnosis, treatment and care for key populations, 2016
update (Geneva, 2016).
96
Chandler et al. (2009).
97
Knapp et al. (2011).
98
UNAIDS, Do no harm – health, human rights and people who use drugs (Geneva, 2016).

22
for governments. These interventions can be cost-effective by most thresholds in the short
term and cost-saving in the long term.
99
Stigma and stigmatizing drug policies affect the effectiveness of drug responses
The stigmatizing attitudes towards people who use drugs that may extend to staff in health
care services can hamper the effectiveness of drug responses, and they are ultimately an
obstacle in achieving SDG Target 10.2 “By 2030, empower and promote the social, economic
and political inclusion of all” and SDG Target 10.3 “Ensure equal opportunity and reduce
inequality of outcome, including by eliminating discriminatory laws, policies and practices and
promoting appropriate legislation, policies and action in this regard”.
Several studies have identified stigma as a significant barrier to accessing health care and
treatment services for drug users. Surveys of health professionals have indicated that they may
hold negative or stereotypical views of people with drug dependence, which are likely to
compromise the provision of high-quality care, while studies of nurses found that negative and
punitive attitudes towards people who use drugs can be relatively common. Judgmental,
unsympathetic or hostile attitudes and views held by health professionals are likely to
discourage individuals with drug-related problems from accessing health care services. The
punitive approaches of law enforcement authorities with regard to people who use drugs can
contribute to their marginalization, particularly when those approaches lead to high levels of
incarceration.
100
Stigma can be reinforced by criminal laws and other structural barriers, which can also fuel
violence, exploitation and a climate of fear.
101
Eleven UN agencies have issued a joint statement on ending discrimination in health care
settings, calling on all stakeholders to commit to review punitive laws that have been proven
to have negative health outcomes and that counter established public health evidence,
including laws that criminalize or otherwise prohibit drug use or possession of drugs for
personal use.
102
99
David P. Wilson, Donald Braedon, Andrew J. Shattock, David Wilson, Nicole Fraser-Hurt, “The cost-
effectiveness of harm reduction”, International Journal of Drug Policy, vol. 26, supplement 1 (2015), pp. S5–S11.
100
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).
101
Socías ME, Marshall BD, Arístegui I, Romero M, Cahn P, Kerr T et al., “Factors associated with healthcare
avoidance among transgender women in Argentina”, International Journal for Equity in Health, vol. 13, No. 1
(2014), p. 81.
102
UNAIDS/UNHCR/UNICEF/WFP/UNDP/UNFPA/UN Women/ILO/UNESCO/WHO/IOM/OHCHR, Joint United
Nations Statement on ending discrimination in health care, 27 June 2017. Available at https://www.who.int/
news-room/detail/27-06-2017-joint-united-nations-statement-on-ending-discrimination-in-health-care-settings.

23
3.
Effective law enforcement and protection of vulnerable
communities
3.1 Prevention of drug-related crime
Many of the risk factors associated with crime and violent behaviour are also risk factors of
drug use, and joint interventions targeting overlapping risk factors can be particularly effective.
Risk factors of crime include:
103
individual risk factors (adverse childhood experiences, history
of violent victimization, mental health disorders, involvement with drugs, alcohol, or tobacco,
poor behavioural control, being male, youthful); family risk factors (low parental involvement,
low emotional attachment to parents or caregivers, low parental education and income,
parental substance abuse or criminality, poor family functioning); community risk factors (low
social capital in community, low access to medical care, situational factors, diminished
economic opportunities, high concentrations of poor residents, high level of transiency, high
level of family disruption, low levels of community participation, socially disorganized
neighbourhoods, availability of drugs, association with delinquent peers, involvement in gangs,
social rejection by peers); and societal risk factors (rapid social change, economic inequality,
poverty, weak economic safety nets, poor rule of law and high corruption, culture of violence,
gender inequalities, high firearm availability, conflict/post-conflict situation). These risk factors
show in particular the close interlinkages between sustainable development and drug matters
as clearly low social development – as related to, for example, SDG 4 (quality education), SDG
8 (economic growth, full and productive employment and decent work) and SDG 10
(inequality) – increases the risk of being involved in drug-related crime and drug use.
A large body of literature, although mostly from developed countries, has established a series
of effective practices to prevent violence and crime (in general, not just drug-related crime),
104
which include: developing safe, stable and nurturing relationships between children and their
parents and caregivers;
105
developing life skills in children and adolescents;
106
hot spot
(data/information-driven) policing, problem-oriented policing, and community policing;
107
community-based responses that improve crime data collection, multisectoral collaboration
and social cohesion;
108
reducing access to firearms and knives (e.g. requiring a license to
possess a gun and bans on purchases of guns by alcoholics appear to reduce rates of both
homicide and robbery);
109
reducing the availability and harmful use of alcohol;
110
promoting
103
WHO, Framework for interpersonal violence prevention (2002); Farrington and Welsh (2007).
104
See e.g. WHO/UNODC/UNDP, Global Status Report on Violence Reduction (2014), and web portals that
contain good practices on crime prevention such as https://campbellcollaboration.org/.
105
See e.g. the UNODC’s Strengthening Families Programme on drug use prevention, which also targets risk
factors of crime.
106
See e.g. Elmira Prenatal Home Visitations (US), and the UNODC’s Line Up, Live Up initiative.
107
See e.g. Silveira, A, Assunção, R, Silva, B and Beato, C, “Impacto do Programa Fica Vivo”, Revista de Saúde
Pública vol. 44, No. 3 (2010) pp. 496–502.
108
See e.g. the Cardiff Model on sharing of anonymized data between hospitals and the police, with up to 42 per
cent reduction in violent injuries; Cure Violence on the use of mediators to de-escalate gang violence and reduce
homicides; and Communities That Care.
109
Kleck, Gary & Kovandzic, Tomislav & Bellows, Jon, “Does Gun Control Reduce Violent Crime?”, Criminal
Justice Review, vol. 41 (2016), pp. 488–513.
110
WHO/UNODC/UNDP, Global Status Report on Violence Reduction (2014).
24
gender equality to prevent violence against women;
111
changing cultural and social norms that
support violence (through long-term community engagement and IEC, not one-off campaigns);
victim identification, care and support programmes (to reduce re-victimization); and
environmental design that reduces the opportunities for crime.
112
An aspect related to the prevention of illicit cultivation is linked to inclusive and sustainable
economic growth, and other income opportunities related to drug production and
transportation in impacted zones (targets related to SDG 8).
3.2 Response to drug-related crime
Criminal justice response to drug
-
related crime:
global
estimates
(2017)
Persons arrested/suspected of drug
possession
1.9 million
Persons arrested/suspected of drug
trafficking
1.2 million
Persons convicted for drug possession
for
personal use
860,000
44 per cent of those
arrested for drug
possession for
personal use
Persons convicted for drug trafficking
740,000
60 per cent of those
arrested for drug
trafficking
Number of persons in prison who were
sentenced for drug possession for personal
use as the principle offence
470,000 4 per cent of all
prison population
Number of persons in prison who were
sentenced for drug trafficking as the
principle offence
1.7 million 16 per cent of all
prison population
Among all persons in prison for any drug-
related offence:
percentage
sentenced for drug
possession for personal use
21
per cent
of all
prisoners sentenced
for drug-related
offences
percentage
sentenced for drug
trafficking
79
per cent
of all
prisoners sentenced
for drug-related
offences
Source: United Nations Survey of Crime Trends and Operations of Criminal Justice Systems (various years).
111 UNODC, Global Study on Homicide Booklet: Gender-related killing of women and girls (2018).
112 Ha, Taehoon; Oh, Gyeong-Seok and Park, Hyeon-Ho, “Comparative analysis of defensible space in CPTED
housing and non-CPTED housing”, International Journal of Law, Crime and Justice vol. 43, No. 4, (2015); Bea,
David C., “Transport engineering and reduction in crime: The Medellín case,” Transportation Research Procedia,
vol. 18. (2016); Cerda, Magdalena et al., “Reducing violence by transforming neighbourhoods: A natural
experiment in Medellín, Colombia”, American Journal of Epidemiology, vol. 175, No. 10 (2012).

25
Data on the number of persons at the various stages of the criminal justice system
(arrested/suspected, convicted and imprisoned) for drug possession for personal use and drug
trafficking are available for only a limited number of countries, and show strong regional
variations.
113
The international drug control conventions do not require Parties to criminalize drug use for
non-medical or non-scientific purposes per se.
114
Subject to constitutional principles and basic
principles of each Party’s legal system, States parties are required to establish as a criminal
offence the cultivation, possession and purchase for personal consumption of controlled drugs
for other than medical and scientific purposes. Criminalization of drug use and possession for
personal use for purposes other than medical and scientific may lead to an increased risk of
illness among people who use drugs and a negative effect on HIV prevention and treatment. It
can increase stigma and discrimination, police harassment and arbitrary arrests. Higher rates
of legal repression have been associated with higher HIV prevalence among people who use
injecting drugs, without a decrease in prevalence of injecting drug use. This is a likely the result
of individuals adopting riskier injection practices out of fear of arrest or punishment.
115
Of the
118 countries that report to UNAIDS, national authorities of 10 countries and civil society
organizations of 16 countries reported that possession of a needle or syringe without a
prescription can be used as evidence of drug use or cause of arrest.
116,
117,
118
The basic principles of the rule of law and access to justice, as also embedded in SDG 16
“Promote peaceful and inclusive societies for sustainable development, provide access to
justice for all and build effective, accountable and inclusive institutions at all levels”, require
the criminal justice response to drug-related crime to be transparent, avoiding arbitrariness
and consistent with international human rights norms and standards.
119
For States to be
consistent with their human rights obligations, they need to make concerted efforts to
combat impunity by conducting prompt, independent, impartial and effective investigations
113
United Nations Survey of Crime Trends and Operations of Criminal Justice Systems (various years).
114
According to the 1988 Convention: “Subject to its constitutional principles and the basic concepts of its legal
system, each Party shall adopt such measures as may be necessary to establish as a criminal offence under its
domestic law, when committed intentionally, the possession, purchase or cultivation of narcotic drugs or
psychotropic substances for personal consumption contrary to the provisions of the 1961 Convention, the 1961
Convention as amended or the 1971 Convention.” article 3(2). The International Narcotics Control Board has
explained “the international drug control treaties do grant some latitude with regard to the penalization of
personal consumption-related offenses. Parties to the 1961 Convention are under an obligation not to permit
the possession of drugs for personal non-medical consumption. Parties to the 1988 Convention are required to
establish as criminal offenses activities preparatory to personal consumption, subject to each party’s
constitutional principles and the basic concepts of its legal system.”
115
A/65/255, para. 26.
116
NCPI data. Available at http://www.aidsinfoonline.org/ncpi/libraries/aspx/Home.aspx; Benoit C, McCarthy B,
Jansson M, “Stigma, sex work, and substance use: a comparative analysis”, Sociology of Health & Illness, vol. 37,
No. 3 (2015), pp. 437–51.; DeBeck K, Cheng T, Montaner JS, Beyrer C, Elliott R, Sherman S et al., “HIV and the
criminalization of drug use among people who inject drugs: A systematic review”, The Lancet HIV, vol. 4, (2017),
pp. e357–e374; see also A/HRC/39/39.
117
Bourmont M, David S, “Hidden victims of war on drugs”, Phnom Penh Post, 24 February 2017. Available at
http://www.phnompenhpost.com/national/hidden-victims-wardrugs.
118
DeBeck K, Cheng T, Montaner JS, Beyrer C, Elliott R, Sherman S et al., “HIV and the criminalization of drug use
among people who inject drugs: A systematic review”, The Lancet HIV, vol. 4, (2017), pp. e357–e374.
119
Report of the Secretary-General to the Security Council: The rule of law and transitional justice in conflict and
post-conflict societies (S/2004/616).

26
into serious human rights violations and bringing alleged perpetrators to justice. At the same
time, States need to protect the rights of people in criminal proceedings, whether they are
victims, witnesses, alleged offenders or prisoners. Law enforcement officials also should
always adhere to the Basic Principles on the Use of Force and Firearms by Law Enforcement
Officials.
120
According to the Human Rights Council’s Working Group on Arbitrary Detention, arbitrary
detention for drug offences or drug use can occur across criminal and administrative settings,
particularly when procedural safeguards are absent, causing a disproportionate impact on
women, children, minority groups and people who use drugs.
121
For example, women who
inject drugs have reported high rates of sexual violence from police and law enforcement
agencies.
122
Structural changes in legislation and law enforcement practices can facilitate the delivery of
services, including minimizing the adverse consequence of drug use.
123
3.3 Countering trafficking in narcotic drugs and psychotropic substances
The achievement of SDG 16, particularly Target 16.4 “By 2030, significantly reduce illicit
financial and arms flows, strengthen the recovery and return of stolen assets and combat all
forms of organized crime”, is at the core of the response to countering drug trafficking
organizations. Vulnerability of one group offers a profit opportunity to another. Organized
criminal groups have always been resourceful in adapting to change in the markets and in their
aim to avoid risk of interception. Hierarchical structures have a major weakness: they can be
easily dismantled when detected by the authorities. As a result, some hierarchical crime groups
have reshaped their structures in recent decades to become networked organizations.
Although most identified international organized criminal groups in the European Union
remain hierarchically organized,
124
Europol suggests a trend away from vertical structures
towards horizontal criminal groups operating along a networked organization model (cellular
120
A/HRC/39/39, paras. 92, 93.
121
A/HRC/30/36.
122
Azim T, Bontell I, Strathdee SA, “Women, drugs and HIV”, International Journal of Drug Policy, vol. 26, No. 1
(2015), pp. s16–s21; Integrated biological and behavioural surveillance reports, 2012–2016; Integrated
biological and behavioural surveillance reports, 2013–2015; Integrated biological and behavioural surveillance
reports, 2011–2016.
123
Abdul-Quader AS, Feelemyer J, Modi S, Stein ES, Briceno A, Semaan S et al., “Effectiveness of structural-level
needle/syringe programs to reduce HCV and HIV infection among people who inject drugs: A systematic
review”, AIDS and Behavior, vol. 17, No. 9 (2013), pp. 2878–2892.
Csete J, Kamarulzaman A, Kazatchkine M, Altice F, Balicki M, Cepeda J et al., “Public health and international
drug policy: Report of the Johns Hopkins–Lancet Commission on Drug Policy and Health”, The Lancet
Commissions, vol. 387, No. 10026 (2016), pp. 1427–1480.
Fernandes RM, Cary M, Duarte G, Jesus G, Alarcão J, Torre C et al., “Effectiveness of needle and syringe
programmes in people who inject drugs: An overview of systematic reviews,” BMC Public Health, vol. 17, No.
309 (2017).
WHO/UNODC/UNAIDS, Technical guide for countries to set targets for universal access to HIV prevention,
treatment and care for injecting drug users, (Geneva, 2009).
124
Europol, European Union: Serious and Organised Crime Threat Assessment (SOCTA) 2017 (The Hague, 2017).

27
structure and less rigid or permanent hierarchies).
125
Loose criminal networks represented 30–
40 per cent of organized criminal groups identified by Europol in 2017.
126
Where law enforcement agencies lack resources and are prone to corruption and where justice
systems are weak and impunity is prevalent, demands on the police to be more effective in
countering drug trafficking can lead to indiscriminate apprehension of those likely to be
perceived as criminals. This can also lead law enforcement agents to target the types of crime
for which suspects are easier to identify, which tend to be minor drug-related offences rather
than more serious offences such as major drug trafficking and homicide. Zero-tolerance
policies, if not properly implemented, may run the risk of generating violence by stigmatizing
and enabling the abuse of power to be directed against people who use drugs or low-level
players in the drug trafficking chain. This, in turn, can lead to mass imprisonment for low-level
offences or to forced detention of people who use drugs.
127
Strategies that focus on rapidly disrupting drug trafficking organizations and reducing violence
in the short term can sometimes lead to more violence. By the same token, strategies that
tackle the root causes of violence in the medium to long term may have a less discernible
impact on short-term violence reduction.
Research suggests that law enforcement and policing that target the protagonists and
elements of the drug trafficking chain that generate the highest profits and the most violence
are more effective in reducing violence than indiscriminate law enforcement by the authorities.
For example, policing that targets the most violent drug traffickers can reduce violence by
creating a powerful deterrent to violent behaviour. Targeted law enforcement can also entail
strategies that do not focus on arresting low-level players in the drug trafficking chain and thus
tend not to add to mass incarceration problems, which would have little positive (or perhaps
even a negative) impact on violence.
128
The assumption that tougher law enforcement results in higher drug prices and therefore
lowers the availability of drugs in the market is not supported by the empirical evidence. The
small number of scientific studies that attempted to make the case have been reviewed over
the last five years and the findings show that, although prohibition itself raises prices far above
those likely to pertain in legal markets, there is little evidence that raising the risk of arrest,
incarceration or seizure at different levels of the distribution system will raise prices at the
targeted level, let alone retail prices.
129
Drug seizures themselves cannot generally be expected
to disrupt drug markets unless they are extremely large since usually suppliers can easily
replace the lost drugs at wholesale costs. If the seizure is associated with dismantling an
organization that had a substantial share of market throughput capacity, then one might
125
Europol, European Union: Serious and Organised Crime Threat Assessment (SOCTA) 2013 (The Hague, 2013).
126
Europol, European Union: Serious and Organised Crime Threat Assessment (SOCTA) 2017 (The Hague, 2017).
127
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).
128
Ibid.
129
Harold A. Pollack and Peter Reuter, “Does tougher enforcement make drugs more expensive?”, Addiction,
vol. 109, No. 12 (2014), pp. 1959–1966.

28
observe a correlation between seizures and price changes. However, once a market is
established, there may be little return on an investment in intense law enforcement.
130
Data-driven policing, problem-oriented policing and community policing have been found
more effective approaches to prevent and respond to crime (including drug-related crime).
131
In recent years there have been some alarming tendencies towards a deeper militarization of
the responses by States to counter drug-related crimes. In some instances, this is associated
with the progressive militarization of civilian police forces. Excessive use of force is more likely
to occur when military or special security forces are involved in drug operations. Such
approaches have disproportionately affected vulnerable groups and have repeatedly resulted
in serious human rights violations.
132
3.4 Proportionate and effective policies and responses (including evidence on
alternatives to incarceration and decriminalization/depenalization of drug use)
The international drug control conventions expressly allow the provision of measures such as
treatment and education as alternatives to conviction or punishment for personal
consumption offences and for all other relevant offences in “appropriate cases of a minor
nature”. Examples of this approach are the diversion of minor cases from the criminal justice
system through the exercise of police or prosecutorial discretion, and the use of non-custodial
measures as an alternative to pretrial detention or imprisonment. This is in line with the
international drug control conventions and with the requirements of an effective and human
rights-compliant penal policy.
133
The excessive use of imprisonment for drug-related offences
of a minor nature is indeed ineffective in reducing recidivism, as well as having a
disproportionate effect on the health and well-being of those arrested for minor offences. It
also overburdens criminal justice systems, preventing them from efficiently coping with more
serious crime. The provision of evidence-based treatment and care services to drug-using
offenders, as an alternative to incarceration, has been shown to substantially increase recovery
and reduce recidivism.
134
Even the most costly forms of alternative interventions (such as drug
courts, though care must be taken to ensure such alternatives do not result in forced treatment)
are more cost-effective than imprisonment, although those approaches require effective
coordination between the health and justice systems.
135
Overuse of imprisonment for minor
130
Jonathan P. Caulkins and Peter Reuter, “How drug enforcement affects drug prices,” Crime and Justice, vol.
39 (2010), pp. 213–271.
131
See e.g. Silveira, A, Assunção, R, Silva, B and Beato, C, “Impacto do Programa Fica Vivo”, Revista de Saúde
Pública, vol. 44, No. 3 (2010), pp. 496–502.
132
A/HRC/39/39, para. 27.
133
See article 36, para. 1 (a) of the 1961 Convention as amended by the 1972 Protocol; article 22, para. 1 (a) of
the 1971 Convention; and article 4 (a) of the 1988 Convention.
134
See Commission on Narcotic Drugs, resolution 55/12. See also UNODC, Introductory Handbook on the
Prevention of Recidivism and the Social Reintegration of Offenders, Criminal Justice Handbook Series (Vienna,
2012), p. 43.
135
See Commission on Narcotic Drugs resolution 58/5: “Supporting the collaboration of public health and justice
authorities in pursuing alternative measures to conviction or punishment for appropriate drug-related offences
of a minor nature”; and resolution 60/6: “Intensifying coordination and cooperation among United Nations

29
drug-related cases may lead to overcrowding and to the infringement of the human rights of
those imprisoned, and may exacerbate the transmission of HIV and other diseases among
people who inject drugs.
In many States, low-level offences such as small-scale drug dealing or trafficking are punished
with harsher penalties than other serious crimes, raising questions about proportionate
sentencing.
136
The United Nations Standard Minimum Rules for Non-custodial Measures (the Tokyo Rules)
137
encourage the use of non-custodial measures at all stages of criminal proceedings, including
diversion and alternatives to pretrial detention, as well as alternatives to imprisonment at the
sentencing and post-sentencing stages. They highlight that non-custodial measures serve to
reduce overcrowding and to meet more effectively the social reintegration needs of offenders
in the community. The Tokyo Rules recommend a wide range of non-custodial measures,
suitable for different types of offences, which should be applied considering not only the
nature and gravity of the offence but also the personality and background of the offender, the
rights of victims and the protection of society.
An example of a particular group that would benefit from this are the large number of women
offenders worldwide who are imprisoned for minor drug-related offences, often as a result of
manipulation, coercion and poverty. If involved in drug trafficking, women are usually minor
players, their criminal offences often being an outgrowth of their own addiction or due to
poverty and other pressures. A significant number of women are used as drug couriers to
smuggle drugs across borders for small sums of money. They come from disadvantaged
backgrounds and sometimes do not understand the risks involved and implications of the acts
that they agree to perform. In the Bangkok Rules,
138
Rule 61 provides specifically for mitigating
factors to be taken into account when sentencing women, even where the offence may have
been violent or may be considered a grave offence according to national law (e.g. drug
trafficking).
139
Bangkok Rule 64 establishes that non-custodial sentences for pregnant women
and women with dependent children shall be preferred where possible and appropriate.
In appropriate cases in which non-custodial measures and sanctions are used to replace
imprisonment, they contribute directly to the reduction of the prison population. A further
advantage of using alternatives to imprisonment is that they can help reduce reoffending, and
thereby help reduce the prison population in the long term. Numerous studies have shown
that reoffending rates are generally lower in the cases of those sentenced to non-custodial
sanctions, in comparison to imprisonment. Further, recidivism itself can lead to a much higher
entities and relevant domestic sectors, including the health, education and criminal justice sectors, to address
and counter the world drug problem”.
136
A/HRC/39/39.
137
United Nations Standard Minimum Rules for Non-custodial Measures (the Tokyo Rules), adopted by General
Assembly resolution 45/110 of 14 December 1990. Available at https://www.unodc.org/pdf/compendium/
compendium_2006_part_01_03.pdf.
138
United Nations Rules for the Treatment of Women Prisoners and Non-custodial Measures for Women
Offenders (the Bangkok Rules), adopted by the UN General Assembly in December 2010. Available at
https://www.unodc.org/documents/justice-and-prison-reform/Bangkok_Rules_ENG_22032015.pdf.
139
UNODC Handbook on Women and Imprisonment, p. 114.

30
prospect of imprisonment for a second or third offence in some countries, resulting in a self-
perpetuating cycle of imprisonment and release.
140
Alternatives to imprisonment are often more effective at achieving important public safety
objectives, such as greater security for the population, than imprisonment. Properly designed
and implemented, they may infringe less on human rights while costing less in the short and
long term.
141
Consistent with international standards and norms (Tokyo Rules, Bangkok Rules),
a number and variety of non-custodial measures and sanctions have been adopted. These
include ensuring that police and prosecutors have sufficient discretion to divert suitable cases
away from the criminal justice system, diversifying the number of alternatives available at the
pretrial stage and restricting by law the use of pretrial detention. They may also include options
for sentencing authorities to impose non-custodial sanctions instead of prison terms for non-
violent drug-related offences. Legislation that provides for alternatives to incarceration can
better respond to the treatment and social reintegration needs of people who use drugs, such
as those who have substance dependency and mental health care needs.
142
In order to be effective, the types of non-custodial measures used and their duration,
conditions, supervision, treatment process and responses to breaches of conditions should
respond to the individual situation, background, risks and needs of offenders.
143
For example,
140
UNODC Handbook on Strategies to Reduce Overcrowding in Prisons, p. 109.
- Robert L., Maes E., Blokland A.A.J. & Wermink H.T., “‘Virtual’ versus ‘real’ prison: which is best?
Comparing the re-incarceration rates after electronic monitoring and imprisonment in Belgium”, in The
Routledge International Handbook of Life-Course Criminology, Blokland A.A.J, Geest V. van der, eds. (London:
Taylor & Francis Ltd., 2017) pp. 417–435.
- McGuire, James, “‘What Works’ to Reduce Re-offending: 18 Years on”, in What Works in Offender
Rehabilitation: An Evidence-Based Approach to Assessment and Treatment, Leam A. Craig et al., eds.
(Chichester: John Wiley & Sons Ltd., 2013).
- William D Bales and Alex R Piquero, “Assessing the impact of imprisonment on recidivism” Journal of
Experimental Criminology, vol. 8, No. 1 (March 2012), pp. 71–101.
- The Scottish Centre for Crime and Justice, Reducing Reoffending: Review of Selected Countries
(Glasgow, 2012).
- Tonry, Michael, “Community Punishments”, in Reforming Criminal Justice, vol. 4, Erik Luna, ed.
(Phoenix, AZ: Arizona State University, 2017b).
- Wermink H.T., Blokland A.A.J., Nieuwbeerta P., Nagin D. & Tollenaar N., “Comparing the effects of
community service and short-term imprisonment on recidivism: A matched samples approach”, Journal of
Experimental Criminology, vol. 6, No. 3 (2010), pp. 325–349.
- Bartels, L, “The weight of the Sword of Damocles: A reconviction analysis of suspended sentences in
Tasmania”, Australian and New Zealand Journal of Criminology, vol. 42, (2009) pp. 72-101.
- Cid, J., “Is Imprisonment Criminogenic?: A comparative study of recidivism rates between prison and
suspended prison sanctions”, European Journal of Criminology, vol. 6, No. 6 (2009), pp. 459–480.
- Lappi-Seppala, T., “Crime Prevention and Community Sanctions in Scandinavia”. Available at
http://www.unafei.or.jp/english/pdf/RS_No74/No74_06VE_Seppala2.pdf.
- The Matrix Knowledge Group, “The Economic Case for and against Prison”. Available at
http://www.matrixknowledge.co.uk/wp-content/uploads/economic-case-for-and-against-prison.pdf.
- Cocker, S., “Using reconviction data to explore the effectiveness of community penalties in West
Yorkshire”, Report no. 2005/6-5 (West Yorkshire, National Probation Service, 2006).
- Bondeson, U.V., “Global Trends in Corrections”, International Annals of Criminology, vol. 36 (1998), pp.
91–116.
141
UNODC, Handbook of Basic Principles and Promising Practices on Alternatives to Imprisonment, p. 80.
142
UNODC, Handbook on Strategies to Reduce Overcrowding in Prisons, p. 52.
143
See Tokyo Rules.

31
women have specific needs that are often better met in the community. Moreover, people
with drug use disorders require treatment, which can in many cases be provided as an
alternative to conviction or punishment. A review of existing practices in Member States shows
that the range of options to provide treatment as an alternative is broad and includes measures
at the pretrial stage (caution with a diversion to treatment, suspension of the prosecution,
conditional dismissal, conditional bail), at the trial/sentencing stage (conditionally deferred
sentence, conditionally suspended sentence, probation, special courts) and at the post-
sentencing stage (early conditional release or parole).
144
Drug courts, when underpinned by human rights and reasonable assumptions about their role,
scale and limits, are viewed as a small but important piece of a broad diversion-based approach
to drug-involved clients within court systems. While in some countries drug courts have been
viewed as relatively successful, in others they are seen as well-meaning but ultimately failed
experiments and a misdirection of drug treatment efforts towards the criminal justice rather
than the public health system.
145
The application of the death penalty for drug-related offences does not respect the spirit of
the international drug control conventions, and has the potential to become an obstacle to
effective cross-border and international cooperation against drug trafficking, as the exchange
of information and extradition on cases where the suspect may face capital punishment are
prohibited in numerous national laws.
146
In accordance with article 6(2) of the International
Covenant on Civil and Political Rights, States that have not abolished the death penalty may
impose it only for the “most serious crimes”, which has been consistently interpreted by UN
human rights treaty bodies as those involving “intentional killing”.
147
As such, drug offences
must never serve as the basis for the imposition of the death penalty.
148
The International
Narcotics Control Board has encouraged all States that retain the death penalty for drug-
related offences to consider the abolition of the death penalty for drug-related offences.
149
144
See UNODC/WHO, Treatment and Care for People with Drug Use Disorders in Contact with Criminal Justice
System: Alternatives to Conviction or Punishment.
145
John Collins, Winifred Agnew-Pauley and Alexander Soderholm, eds., Rethinking Drug Courts: International
Experiences of a US Policy Export (London School of Economics and Political Science, International Drug Policy
Unit, 2019).
146
Contribution of the Executive Director of the United Nations Office on Drugs and Crime to the high-level
review of the implementation of the Political Declaration and Plan of Action on International Cooperation
towards an Integrated and Balanced Strategy to Counter the World Drug Problem, to be conducted by the
Commission on Narcotic Drugs in 2014.
147
Human Rights Committee, General comment No. 36, CCPR/C/GC/36 (2018), para. 35: “The term ‘the most
serious crimes’ must be read restrictively and appertain only to crimes of extreme gravity, involving intentional
killing. Crimes not resulting directly and intentionally in death, such as attempted murder, corruption and other
economic and political crimes, armed robbery, piracy, abduction, drug and sexual offences, although serious in
nature, can never serve as the basis, within the framework of article 6, for the imposition of the death penalty.”
148
Ibid.; see also A/73/260 paras. 24–27, 63, and A/HRC/739/39, paras. 59, 91.
149
See International Narcotics Control Board, “INCB reiterates its call to States to consider the abolition of the
death penalty for drug-related offences”, press release, 1 August 2016. Available at http://www.incb.org/incb/
en/news/press-releases/2016/press_release010816.html; Viroj Sumyai, President, International Narcotics
Control Board, “Item 5 (c) Implementation of the international drug control treaties: International Narcotics
Control Board”, statement at the sixty-first session of the Commission on Narcotic Drugs, 14 March 2018.
Available at http://www.incb. org/documents/Speeches/Speeches2018/Speech.

32
3.5 Legal guarantees and safeguards pertaining to criminal justice proceedings and the
justice sector (including legal aid and the right to a fair trial)
A central aspect of the 2030 Agenda is the concept of “leaving no one behind” and ensuring
that those who are furthest behind are reached first. SDG Target 16.3 highlights the rule of law
and equal access to justice, calling on countries to “promote the rule of law at the national and
international levels and ensure equal access to justice for all”. Access to legal aid is
fundamental in this regard, to ensure a criminal justice system is fair, humane, efficient and
based on the rule of law, which can reduce the length of time suspects are held in custody and
pretrial detention, congestion in the courts, wrongful convictions and prison overcrowding,
while also being able to improve the conditions of prisoners serving their sentence and reduce
rates of reoffending and victimization. Persons who are in contact with the criminal justice
system because of drug offences, and persons living with HIV and other serious contagious
diseases, are particularly vulnerable in this context. The UN Principles and Guidelines on Access
to Legal Aid in Criminal Justice Systems
150
specify in Principle 10 that special measures should
be taken to ensure meaningful access to legal aid for drug users and persons living with HIV
and other serious contagious diseases. However, Member States have not reported on the
availability of these specialized services,
151
while progress is visible regarding provision of
services for children, persons with disabilities, and women.
The large volume of drug-related offences for personal possession and drug use has led some
States to seek methods to move cases more quickly through the criminal justice system. This
has resulted in growth of the use of “trial waiver” systems. Although trial waiver systems do
succeed in moving multiple cases through criminal justice systems, the price is often less
procedural protection and judicial oversight.
152
3.6 Addressing links between drug trafficking and peace and security (money-
laundering, corruption, armed conflict, and political fragility and stability)
The drug trade has been a significant source of income for some terrorist, insurgent and non-
State armed groups, while for others it has been one of many revenue streams or it may hardly
have played a role at all. The most comprehensive evidence linking the terrorist groups on
which the Security Council has imposed sanctions with the drug trade relates to the Taliban.
The group has taxed entities involved in illicit drug production, manufacture and trafficking,
and it has been directly involved in drug trafficking.
153
UNODC estimated that terrorist and
150
UNODC, United Nations Principles and Guidelines on Access to Legal Aid in Criminal Justice Systems (2013)..
151
UNDP/UNODC, Global Study on Legal Aid – Global Report (2016).
152
A/HRC/39/39, para. 37.
153
Security Council, “Letter dated 18 August 2015 from the Chair of the Security Council Committee established
pursuant to resolution 1988 (2011) addressed to the President of the Security Council” (26 August 2015);
UNODC, The Opium Economy in Afghanistan: An International Problem (New York, 2003); UNODC, Addiction,
Crime and Insurgency: The Transnational Threat of Afghan Opium (Vienna, 2009); UNODC, The Global Afghan
Opium Trade: A Threat Assessment (Vienna, July 2011).

33
insurgent groups raised about US$150 million in 2016 from the Afghan opiate trade in taxes
levied on the cultivation of opium poppy and trafficking of opiates.
154
In contexts where drug trafficking syndicates or armed groups funded through drug money
operate, these groups’ economic and coercive power has in several contexts quickly translated
into political influence, undermining the integrity of state institutions and longer-term
peacebuilding prospects, undermining the achievement of SDG 16, particularly Target 16.3
“Promote the rule of law at the national and international levels and ensure equal access to
justice for all”.
155
Drug trafficking also fuels corruption, going against SDG Target 16.5 “Substantially reduce
corruption and bribery in all their forms”. Drug trafficking is extremely lucrative, making
corruption of high-level and local level officials a prime vector for exercising political
influence.
156
Opportunities for corruption exist at every stage of the drug production and supply chain.
However, more research is needed on how different types of corruption interact with drug
markets.
157
Organized crime and drug trafficking can also contribute directly and indirectly to violent
conflict. The World Bank has identified trafficking in drugs as one of the major international
stressors that need to be mitigated if a country is to move away from fragility and violence.
The UN and World Bank have also argued that drug-related violence can reflect and exacerbate
local grievances that ultimately lead to violent conflict.
Different stages of the drug problem result in different manifestations of violence and can
undermine the achievement of SDG Target 16.1 “Significantly reduce all forms of violence and
related death rates everywhere”. Drug use may lead to violence related to the psychoactive
effects of drugs (psychopharmacological violence), as well as to crime committed in order to
obtain funds for purchasing drugs (economic violence). The intensity of drug-related violence
is greatest, however, when associated with drug trafficking (systemic violence), as the example
of Latin America shows. The traumatic effects of violence can also increase vulnerability to drug
use.
Yet drug trafficking and production do not necessarily produce violence, as illustrated by the
low levels of homicide in transit countries affected by the opiate trafficking routes in Asia.
Characteristics of the market and drug trafficking organizations may explain variations: market
competition can generate violence in illicit markets, while differences in the internal structure
of trafficking networks, which may be characterized by varying degrees of cohesiveness and
hierarchy, can also play a role.
154
UNODC, Sustainable Development in an Opium Production Environment: Afghanistan Opium Survey Report
2016.
155
WB, World Development Report (2011); UN/WB, Pathways for Peace: Inclusive Approaches to Preventing
Violent Conflict (2018).
156
Louise Bosetti, John de Boer, and James Cockayne, “Crime-Proofing Conflict Prevention, Management, and
Peacebuilding: A Review of Emerging Good Practice” (United Nations University, August 2016).
157
UNODC, World Drug Report 2017 (United Nations publication, Sales No. E.17.XI.6).

34
The profits associated with the drug trade are a key motivation for non-State armed groups,
including terrorist organizations, to engage in or facilitate drug trafficking. In a number of
countries, resources generated in illicit markets such as drug markets have played a role in
complicating and extending armed conflicts, often increasing their overall lethality. In general,
the drug trade flourishes where SDG 16, and particularly Targets 16.1–16.6, are far from being
achieved: State presence is weak, where the rule of law is unevenly applied and where
opportunities for corruption exist. At the same time, the wealth and power of drug trafficking
organizations provide them with resources to buy protection from law enforcement agents,
politicians and the business sector, thereby reinforcing corruption and further weakening the
achievement of SDG 16.
158
Billions of dollars flow through the hands of drug trafficking organizations each year, having a
large impact on local and wider economies and polities. Some recent global estimates suggest
that the proceeds of drug sales accounted for slightly more than one quarter of overall
revenues of transnational organized crime groups in 2014, with a maximum range from around
one fifth to one third of such revenues. In recent years, drug-related income seems to have
represented the second largest source of income — after counterfeiting of a broad range of
goods — of transnational organized crime groups at the global level.
159
In the short term, an inflow of drug money can boost investment and local gross domestic
product. But the long-term effects tend to be negative, particularly when drug-related
proceeds comprise a sizeable portion of the total economy of a community or a country.
Studies suggest that an injection of laundered money, including from illicit drug activities, is
associated with reductions in overall annual economic growth rates, particularly in smaller and
less developed countries. One estimate, based on a study of 17 countries of the Organization
for Economic Cooperation and Development, suggests that a US$1 billion increase in money-
laundering could reduce overall economic growth by between 0.03 and 0.06 percentage
points.
160
Profit is generated across the entire chain of drug production and distribution, but it is at the
final stage that it tends to be highest. A UNODC study estimated that almost half of the profit
made along the major heroin trafficking route from Afghanistan to Europe was generated in
the four largest European consumer countries. Nevertheless, the size of the illicit economy
associated with drugs, relative to the licit economy, tends to be higher in drug-producing
countries, partly because of their relatively smaller economies.
161
The proceeds from drug trafficking can also complicate and undermine mediation and
peacemaking efforts. A major source of funding for non-state armed groups in several
contexts, proceeds from drug trafficking often translate into lowered incentives for these
158
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).
159
This was based on drug trafficking estimates of $426 to $652 billion out of a total transnational organized
crime income of $1.6 trillion to $2.2 trillion in 2014, see Channing May, “Transnational crime and the developing
world”, Global Financial Integrity (Washington D.C., March 2017).
160
UNODC, World Drug Report 2017 (United Nations publication, Sales No. E.17.XI.6).
161
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).

35
groups to enter into ceasefire or peace agreements, or other forms of political settlements,
thereby protracting conflicts.
4.
Alternative development
The reasons for cultivating illicit crops are diverse and often specific to particular areas. Illicit
crop cultivation is linked, on the one hand, to the dynamics of cultivation itself and, on the
other hand, to underlying drivers and root causes related to conditions of vulnerability found
in geographical areas where cultivation takes place, such as weak rule of law or a lack of social
and economic development. As survival and subsistence are real considerations for many
households that engage in illicit crop cultivation, they are frequently risk averse and take a
variety of elements into account when they make decisions on narcotic crop cultivation. While
poverty can be a driver of illicit drug cultivation, not all poor farmers are involved in illicit crop
cultivation and not all framers involved in illicit crop cultivation are poor.
Alternative crop cultivation depends on many factors: possession of the requisite skills and
knowledge for growing such crops; geographical and environmental factors, such as climate,
the availability of water and arable land, and proximity to market; household-specific
socioeconomic factors, such as level of income, existing employment opportunities, access to
credit and size of landholding; developmental facilities such as access to roads, the power grid
and educational and health services; and sociopolitical and institutional factors, such as
interception risk, security, government control and rule of law.
162
If development interventions
are not sensitive to the vulnerabilities of communities to specific drug issues, they may
inadvertently trigger dynamics that increase illicit cultivation.
163
Alternative development works when it has a long-term vision based on structural
transformation, adequate funding and the political support to integrate it into a broader
development and human rights agenda. Sustainable results in reducing illicit cultivation in
different communities around the world can be obtained when the socioeconomic
development of communities and the livelihood of rural households are improved. Viable,
sustainable income-generating alternatives need to be available, and decent work
opportunities strengthened, in order to decrease dependence on illicit cultivation over time.
There is a general consensus that alternative development interventions can work only if they
manage to achieve or build on the involvement of local communities or beneficiaries. Many
successful alternative development programmes have a specific focus on women and their
empowerment. Women can play a critical role in increasing the impact of alternative
development.
164
Sequencing alternative development interventions is crucial to ensure that structural
transformation and alternative livelihoods are functioning and providing adequate living and
working conditions before eradication of illicit crops starts.
165
162
UNODC, World Drug Report 2015 (United Nations publication, Sales No. E.15.XI.6).
163
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).
164
UNODC, World Drug Report 2015 (United Nations publication, Sales No. E.15.XI.6).
165
A/HRC/39/39, paras. 79, 80.

36
Despite the amount of attention given to alternative development at the international level,
and its crucial role in realizing SDG 8, there is a disconnect between international rhetoric and
funding. Funding has decreased considerably in the last few years. Overall gross disbursements
of alternative development funds from OECD countries declined by 71 per cent between 2009
and 2013. In 2013, these disbursements accounted for just 0.1 per cent of global development
assistance.
5.
Cross-cutting (or topical) issues
5.1 New psychoactive substances
In recent years, hundreds of NPS have emerged; a total of 803 NPS were reported to UNODC
during the period 2009–2017. However, while the global NPS market remains widely
diversified, with the exception of a few substances, NPS do not seem to have established
themselves on drug markets or replaced traditional drugs on a larger scale.
166
The conditions
are in place for an expansion of the NPS market (in terms of the numbers of substances), but
there has been no sign of significant expansion to date. Most of the harm generated by drug
use comes still from controlled substances (traditional classes) or non-medical use of
prescription drugs rather than from NPS.
Some studies have shown that selected groups of people are particularly vulnerable to NPS.
Patterns of NPS use among marginalized, vulnerable and socially disadvantaged groups,
including homeless people and people with mental health disorders, continue to be
documented in some countries. High levels of use of NPS are reported by prisoners and people
on probation, and this remains an issue of concern in numerous countries in Europe, North
America and Oceania.
167,
168
The proliferation of NPS on the market has led the CND, following recommendations of the
WHO, to prioritize international control of some of those substances. A 2014 UNODC-WHO
Expert Consultation on NPS recognized the need to prioritize the international control of NPS
that are more persistent, prevalent and harmful. The Expert Consultation concluded that a
phased approach to NPS prioritization is required, with the two main criteria for consideration
being evidence of harm (or potential harm) of a substance, and the prevalence (or proxies for
prevalence) of its use.
169
Since 2015, the UN has taken action to place 39 NPS under
international control.
5.2 Non-medical use of pharmaceuticals
The non-medical use of prescription drugs is becoming a major threat around the world.
170
Different pharmaceutical opioids are misused in different regions. In North America, illicitly
166
UNODC, World Drug Report 2018 (United Nations publication, Sales No. E.18.XI.9).
167
UNODC, World Drug Report 2017 (United Nations publication, Sales No. E.17.XI.6).
168
UNODC, World Drug Report 2018 (United Nations publication, Sales No. E.18.XI.9).
169
Report by LSS/RAB/DPA/UNODC, New psychoactive substances: overview of trends, challenges and legal
approaches (E/CN.7/2016/CRP.2).
170
UNODC, World Drug Report 2018 (United Nations publication, Sales No. E.18.XI.9).

37
sourced fentanyl, mixed with heroin or other drugs, is driving the unprecedented number of
overdose deaths.
171
In Europe, the main opioid of concern remains heroin, but the non-medical
use of methadone, buprenorphine and fentanyl has also been reported.
172
In countries in West
and North Africa, and the Near and Middle East, the non-medical use of tramadol, a
pharmaceutical opioid that is not under international control, is emerging as a substance of
concern.
173
The non-medical use of the common sedative/hypnotic benzodiazepines and
similar substances is now one of the main drug use problems in some 60 countries. The misuse
of benzodiazepines carries serious risks, not least an increased risk of overdose when used in
combination with heroin. Benzodiazepines are frequently reported in fatal overdose cases
involving opioids such as methadone.
174
5.3 Use of internet for drug-related activities
Although the scale of drug trafficking on the darknet (that part of the “deep web” containing
information that is only accessible using special web browsers) remains limited, it has shown
signs of rapid growth.
175
Authorities in Europe estimated that drug sales on the darknet from
22 November 2011 to 16 February 2015 amounted to roughly US$44 million per year.
176
However, a later study estimated that, in early 2016, drug sales on the darknet were between
$14 million and $25 million per month, equivalent to between $170 million and $300 million
per year.
177
5.4 Social inclusion
Marginalization can be viewed as contributing to illicit drug use, just as drug use can be viewed
as contributing to the marginalization of some users: drug use can cause a deterioration in
living conditions, while processes of social marginalization can be a reason for initiating drug
use. Several risk factors for marginalization have been shown to be linked to drug use, including
unemployment, homelessness, incarceration, sex work and vulnerable youth (such as young
victims of family abuse and violence).
In some societies, the stigma of being drug users and
discrimination drive people who use drugs to the margins of society. People with drug use
disorders are frequently distanced from their communities and families. The marginalization
and stigmatization of people who regularly use drugs also have a negative impact on their
employment opportunities and social relationships.
178, 179
171
Holly Hedegaard, Arialdi M. Miniño, and Margaret Warner, “Drug Overdose Deaths in the United States,
1999–2017”, NCHS Data Brief, No. 329 (November 2018).
172
EMCDDA, European Drug Report 2017: Trends and Developments.
173
UNODC, World Drug Report 2018 (United Nations publication, Sales No. E.18.XI.9).
174
Ibid.
175
Ibid.
176
EMCDDA/Europol, Drugs and the Darknet: Perspectives for Enforcement, Research and Policy, Joint
publications series (Luxembourg: Publications Office of the European Union, 2017).
177
Rand Europe, “Internet-facilitated drugs trade: An analysis of the size, scope and the role of the Netherlands”
(2016).
178
EMCDDA, Annual Report 2003: The State of the Drugs Problem in the European Union and Norway (Lisbon,
2003).
179
UNODC, World Drug Report 2016 (United Nations publication, Sales No. E.16.XI.7).

38
5.5 Information (monitoring, epidemiology and statistics)
Investment in data and evidence-based research pays off in more effective and efficient
policies. In countries where adequate investments in data collection, research, monitoring and
evaluation have been made and systems of government and civil society have been enhanced,
more strategic, effective and efficient responses to illicit drug use and supply have been put in
place. Up-to-date, comprehensive, disaggregated and transparent data are essential tools to
understand drug use, its impact on health and development, drug supply, the dynamics of drug
markets, and to evaluate drug control efforts. Data and analysis can measure the impact of
illicit drug use, supply and drug control efforts on the enjoyment of human rights. Various tools
are available to improve data and indicators. UNODC, WHO and UNAIDS have developed
standards on drug epidemiology and drug supply and trafficking. OHCHR has also developed a
set of human rights indicators for the realization of human rights,
180
and guidance on a human
rights-based approach to data collection in the implementation of the Sustainable
Development Goals.
181
All these tools – together with the multitude of statistical standards –
can provide guidance in strengthening and streamlining existing data collection and analysis
tools in drug control efforts.
6.
Treaties and resolutions on international drug policy
The three international drug control conventions regulate international policy on drugs. They
are the 1961 Single Convention on Narcotic Drugs (with the 1972 Protocol to underscore, inter
alia, the need to provide adequate prevention, treatment and rehabilitation services); the
Convention on Psychotropic Substances of 1971; and the United Nations Convention against
Illicit Traffic in Narcotic Drugs and Psychotropic Substances of 1988. Member States reiterated
at many occasions, most recently in the UNGASS 2016 outcome document that those three
conventions, whose ultimate goal is to ensure the health, safety and well-being of all humanity,
together with other international instruments, including in particular human rights treaties,
constitute the cornerstone of the international drug control system. The General Assembly has
consistently adopted resolutions declaring that international drug control must be carried out
in conformity with the Charter, and “with full respect for human rights” (see resolutions
A/RES/71/211, A/RES/72/198, A/RES/ 73/192; A/HRC/; see also UNGASS 2016).
Beyond international treaties, international drug policy has evolved over the years through a
series of resolutions, action plans and outcome documents agreed by different organs of the
UN system. The CND, as the principal policymaking body of the UN with prime responsibility
for drug-related matters, has over the past decade adopted over 120 resolutions covering a
wide range of issues, including: prevention, treatment and care, HIV-AIDS prevention, and
other health-related issues; promoting non-stigmatizing attitudes; the availability of and
access to health services; enhancing the availability of controlled substances for medical and
scientific purposes. Mainstreaming a gender perspective as well as implementing policies
tailored to the specific needs of the most vulnerable members of society, including children
and youth, were core elements in the resolutions adopted over the past decade. In
180
See www.ohchr.org/EN/Issues/Indicators/Pages/documents.aspx.
181
See www.ohchr.org/EN/NewsEvents/Pages/DataForSustainableDevelopment.aspx.

39
addressing persistent and emerging challenges, the CND also approved resolutions on
preventing and responding to the adverse health consequences and risks associated with the
use of new psychoactive substances; on addressing the challenges posed by the non-medical
use of synthetic opioids; and on the illicit trafficking of precursors and non-scheduled
precursor chemicals. Other key topics such as promoting proportionate and effective policies,
including alternatives to incarceration; preventing and countering of drug-related crime;
addressing links with other forms of organized crime as well as socio-economic issues were as
well addressed in Commission’s resolutions adopted during the last decade. On alternative
development, the UN General Assembly and the CND have recognized that one of the drivers
of illegal cultivation is poverty and lack of socioeconomic opportunities and repeatedly
reaffirmed the commitment to address these root causes of illicit drug crop cultivation,
including by tackling poverty and creating sustainable livelihood opportunities.
182
In addition to its resolutions, a number of which were recommended for adoption by the
Economic and Social Council and the General Assembly, the Commission has in the past decade
adopted three main policy documents: following review of the progress made in the
implementation of the declarations and action plans adopted by the special session of the
General Assembly in June 1998, the Commission on Narcotic Drugs adopted in March 2009 the
Political Declaration and Plan of Action on International Cooperation towards an Integrated
and Balanced Strategy to Counter the World Drug Problem, based on three pillars – demand
reduction, supply reduction and international cooperation – and establishing 2019 as target
date for the commitments made in operative paragraph 36. A high-level review was held in
2014, resulting in the adoption of the 2014 Joint Ministerial Statement. Shortly thereafter, the
General Assembly tasked the Commission to lead an open-ended and inclusive preparatory
process for the Special Session on the World Drug Problem (UNGASS) held in April 2016, at
which occasion the General Assembly adopted unanimously the outcome document “Our joint
commitment to effectively addressing and countering the world drug problem”, which had
been negotiated within the CND and which represents the most recent international consensus
in drug policy.
The UNGASS outcome document promotes a more comprehensive understanding of the world
drug problem, with a number of issues that received less attention in previous documents. The
outcome document demonstrates that health-related issues have come to play a more
important role on the agenda of the CND, with topics of prevention of drug abuse, treatment
and care as standing items on the work programme of the Commission, which is also reflected
in the composition of the delegations at the Commissions’ meetings. The UNGASS outcome
document recognizes that efforts to achieve the 2030 Agenda for Sustainable Development
and to effectively address the world drug problem were complementary and mutually
reinforcing. Member States for the first time included a whole chapter on the importance of
182
See e.g. General Assembly resolution 68/196, United Nations Guiding Principles on Alternative Development
(11 February 2014), A/RES/68/196, paras. 10, 16, 18 (a, c, p); General Assembly resolution S-30/1, Our joint
commitment to effectively addressing and countering the world drug problem (4 May 2016), A/RES/S-30/1,
annex, para. 7; UNODC, World Drug Report, pp. 77–81; Economic and Social Council resolution 2017/20,
Promoting the implementation of the United Nations Guiding Principles on Alternative Development and related
commitments on alternative development and regional, interregional and international cooperation on
development-oriented, balanced drug control policy addressing socioeconomic issues (23 July 2017),
E/RES/2017/20, paras. 4, 5, 11, 25, 26, 29.

40
ensuring the availability of and access to controlled substances for medical and scientific
purposes, including for the relief of suffering and pain. The document recognizes the
importance of supply reduction and the need for criminal justice and law enforcement
responses that adhere to principles of proportionality and the rule of law, and it further
highlights persistent and emerging challenges, including new psychoactive substances, opioid
overdoses and the use of the internet for drug-related activities. Member States also agreed
on a set of recommendations on drugs and human rights, youth, children, women and
communities, underscoring the importance of mainstreaming issues of gender and youth into
drug-related policies and programmes. In addition, drug-related socioeconomic issues are
covered within the document, which calls for long-term, comprehensive and sustainable
development-oriented and balanced drug control policies and programmes. Other
Commissions and UN bodies have agreed on recommendations and resolutions relevant to
drugs.
The General Assembly, the Human Rights Council, the Committee on Economic, Social and
Cultural Rights, the Committee on the Rights of the Child, the Committee on the Elimination of
Discrimination against Women, the Special Rapporteur on the right of everyone to the
enjoyment of the highest attainable standard of physical and mental health and the Special
Rapporteur on torture and other cruel, inhuman or degrading treatment or punishment have
all considered that measures to minimize the adverse health consequences of drug use are
essential for people who use drugs.
183
The United Nations Committee on the Elimination of Discrimination against Women, for
example, has addressed drug issues and women on several occasions. The Committee
recommended to provide health and counselling support to women with drug addiction in line
with general recommendation No. 24 (1999) on women and health,
184
and to ensure gender-
sensitive and evidence-based drug treatment services to reduce harmful effects for women
who used drugs. The Committee has also expressed concerns about the excessive use of
incarceration as a drug control measure against women and the ensuing female
overpopulation in prison.
185
United Nations human rights mechanisms have reviewed a number of issues related to drugs.
They have expressed concern about the unnecessary and disproportionate use of the criminal
justice system for drug-related offences
186
and the CND
187
has provided guidance on the
promotion of proportionate sentencing for drug-related offences of an appropriate nature in
implementing drug control policies. According to the OHCHR, proportionate sentencing is also
relevant to pretrial detention for drug cases.
188
The Convention against Torture and Other
Cruel, Inhuman or Degrading Treatment or Punishment states that pretrial detention can be
183
A/HRC/39/39, para 17.
184
A/54/38/Rev.1, chap.1. Available at https://tbinternet.ohchr.org/Treaties/CEDAW/Shared%20Documents/
1_Global/INT_CEDAW_GEC_4738_E.pdf
185
CEDAW/C/LKA/CO/8; CEDAW/C/CAN/CO/8-9; CEDAW/C/UKR/CO/8; CEDAW/C/KGZ/CO/4;
CEDAW/C/GEO/CO/4-5.
186
A/HRC39/39, CAT/C/BLR/CO/5.
187
Commission on Narcotic Drugs, resolution 59/6.
188
A/HRC/39/39, para 58; see also CAT/OP/BEN/1.

41
used only as a last resort “for the shortest time possible, and only for the most serious
offences”.
189
The International Covenant on Civil and Political Rights has stated the right to equality before
courts and tribunals and to a fair trial as a key element of human rights protection. The right
to be presumed innocent until proved guilty according to law is an essential element of the
right to a fair trial.
190
The report of the High Commissioner for Human Rights to the Human Rights Council provided
some practical examples of what may constitute a human rights violation in the criminal justice
response to drug-related crime: the use of legal presumptions in some countries, whereby
persons found with amounts of drugs above specified thresholds, or in possession of keys to a
building or vehicle where drugs have been found, are presumed to be guilty of drug trafficking,
has been condemned as reversing the burden of proof in criminal proceedings, and may
amount to a violation of the right to a fair trial.
191
In accordance with the Human Rights Committee, physical and mental pain and suffering
associated with withdrawal symptoms may amount to torture or ill-treatment.
192
The
Committee against torture discouraged the use of solitary confinement as a “management
method” in compulsory isolation drug treatment centres.
193
Several international human rights mechanisms, as well as 11 UN entities, considered that a
major obstacle to accessibility of treatment is the criminalization of personal use and
possession of drugs for other than medical and scientific purposes, and recommended that
consideration be given to removing obstacles to the right to health, including by refraining
from imposing criminal penalties for the personal use and possession of drugs, within the
flexibility allowed by the international drug control conventions.
194
The Committee on Economic, Social and Cultural Rights,
195
the Special Rapporteurs on the right
to health; on freedom from torture and other ill-treatment; and on extrajudicial, summary or
189
CAT/C/54/2.
190
International Covenant on Civil and Political Rights, article 14.
191
A/HRC/39/39, para. 36.
192
CCPR/C/RUS/CO/7.
193
CAT/C/CHN/CO/5.
194
CESCR, Concluding Observations, Philippines, E/C.12/PHL/CO/5-6 (2016), para. 54; A/65/255; Report to the
General Assembly by UN Special Rapporteur on the right to health, Anand Grover (2010), A/65/255, para. 72;
Report of the United Nations High Commissioner for Human Rights: Study on the impact of the world drug
problem on the enjoyment of human rights, 4 September 2015, A/HRC/30/65.
UNAIDS/UNHCR/UNICEF/WFP/UNDP/UNFPA/UN Women/ILO/UNESCO/WHO/IOM/OHCHR, Joint United Nations
Statement on ending discrimination in health care, 27 June 2017; A/HRC/39/39, paras. 14–17.
195
CESCR, Concluding Observations, Philippines (2016), E/C.12/PHL/CO/5-6, para. 54.

42
arbitrary executions;
196
the Committee on the Rights of the Child;
197
and the Office of the
United Nations High Commissioner for Human Rights
198
have recommended the
decriminalization of drug use and possession for personal use as an important step towards
fulfilling the rights to health and towards protecting the safety and well-being of communities.
Twelve UN agencies have jointly recommended reviewing and repealing laws criminalizing drug
use and the possession of drugs for personal use.
199
The World Health Organization has
recommended that countries work towards the decriminalization of drug use as a strategy to
reduce incarceration and support access to HIV-related services for people who use drugs.
200
With regard to the eradication of illicit crops, international human rights mechanisms have
emphasized that it should not negatively affect the environment or the health and welfare of
farmers, their families or other stakeholders. International human rights mechanisms objected
to aerial spraying for crop eradication because of the harm it can cause to farmers and their
children, as well as to environment.
201
7.
Concluding observations
From the UN’s experience over the last decade, it is clear that the multifaceted nature of the
problem requires a comprehensive, multidisciplinary approach that includes targeted law
enforcement efforts to dismantle organized crime and ensure the physical security of people,
alongside efforts that promote health, good governance and sustainable development
underpinned by the drug control conventions, human rights laws, principles and standards,
such as the principles of equality and non-discrimination. Let us not forget that the health and
welfare of humankind are the fundamental underpinnings of the three international drug
control conventions, which form the cornerstone of the international drug control system. The
drug control conventions therefore allow countries sufficient flexibility to design and
implement national drug policies according to their priorities and needs, consistent with the
principle of common and shared responsibility. As emphasized by UNGASS, the 2030 Agenda
for Sustainable Development and the international drug control conventions, international
human rights treaties and other relevant instruments are complementary and mutually
reinforcing.
The UN system remains committed to supporting Member States in developing and
implementing truly balanced, comprehensive, integrated, evidence-based, human rights-
196
Office of the High Commissioner for Human Rights (15 April 2016), Joint Open Letter by the UN Working Group
on Arbitrary Detention; the Special Rapporteurs on extrajudicial, summary or arbitrary executions; torture and
other cruel, inhuman or degrading treatment or punishment; the right of everyone to the highest attainable
standard of mental and physical health; and the Committee on the Rights of the Child, on the occasion of the
United Nation General Assembly Special Session on Drugs. Available at https://www.ohchr.org/
Documents/Issues/Health/UNGASS-joint_OL_HR_mechanisms_April2016.pdf
197
Ibid.
198
Report of the United Nations High Commissioner for Human Rights: Study on the impact of the world drug
problem on the enjoyment of human rights, 4 September 2015, A/HRC/30/65.
199
UNAIDS/UNHCR/UNICEF/WFP/UNDP/UNFPA/UN Women/ILO/UNESCO/WHO/IOM/OHCHR, Joint United
Nations Statement on ending discrimination in health care, 27 June 2017.
200
WHO, Consolidated guidelines on HIV prevention, diagnosis, treatment and care for key populations (2014);
see also UNODC, Handbook on strategies to reduce overcrowding in prisons (2013), pp. 29–30 and 55–57.
201
See CRC/C/COL/CO/3, A/HRC/4/32/Add.2, A/HRC/7/11/Add.3 and A/HRC/4/30/Add.1.

43
based, development-oriented and sustainable responses to the world drug problem, within
the framework of the 2030 Agenda for Sustainable Development, and as envisaged by the
operational chapters of the UNGASS outcome document. By working together through the
Task Team (the “UN system coordination Task Team on the Implementation of the UN System
Common Position on drug-related matters”), the UN system can provide the kind of
multidisciplinary support to Member States that can deliver more effective, evidence-based
and humane drug control policies that help rather than hinder a country’s efforts to achieve
its Sustainable Development Goals and to “leave no one behind”. For more information on
these latest efforts by the UN system to better support Member States, please see the UN
System Common Position adopted in November 2018 to support the implementation of the
international drug control policy through effective inter-agency collaboration (Annex I); the
summary of key messages resulting from the knowledge produced and acquired by the UN
system on drug-related matters (Annex II); and the examples of existing joint programmes
between UN entities on drug-related matters (Annex III). Going forward, on the basis of the
evidence produced in this brief, the members of the Task Team
202
will continue to work
together to produce evidence-based briefs on the links between drug policies and sustainable
development, and to deliver integrated assistance through joint programmes. This can support
Member States in designing and implementing effective drug policies that meet international
standards and obligations. As highlighted by the Secretary General, the Task Team encourages
interested donors to provide support to its work, so that it can continue to produce tailor-
made evidence in support of the needs of Member States, as well as continue to deliver
integrated assistance through its existing joint programmes and through new kinds of
partnerships.
202
Current membership of the Task Team: UNODC, UNDP, OHCHR, UNAIDS, WHO, DPPA, UNESCO, UN Women,
UNICEF, UN-Habitat, ECLAC, ILO, ICAO, IMO, UPU and UNU.

44
Annex I
United Nations system common position supporting the
implementation of the international drug control policy through
effective inter-agency collaboration
203
Shared principles
Reiterating our strong commitment to supporting Member States in developing and
implementing truly balanced, comprehensive, integrated, evidence-based, human rights-
based, development-oriented, and sustainable responses to the world drug problem, within
the framework of the 2030 Agenda for Sustainable Development, we, the members of the
United Nations system, underline the importance of the following common values:
• We commit to supporting the practical implementation of the outcome of the 2016
United Nations General Assembly Special Session (UNGASS) in April 2016 as a
blueprint for action, charting a path that promotes more effective and humane drug
control policies, supporting the Sustainable Development Goals’ commitments to
leave no one behind;
• We recognize that the world drug problem is complex and multifaceted and that
challenges posed by drugs have wide-ranging adverse impacts on security, human
rights and development;
• We underscore that the multifaceted nature of the problem requires a
comprehensive approach that includes law enforcement efforts ensuring people’s
security as well as efforts promoting health, human rights, including equality and
non-discrimination, and sustainable development;
• We commit to promoting a truly evidence-based, balanced approach, whereby
sufficient attention is given to measures that address the root causes of drug abuse,
cultivation and other involvement in the drug trade;
• We acknowledge that we have a common and shared responsibility to work
together, particularly through the Commission on Narcotic Drugs (CND), to pursue a
coordinated, balanced and comprehensive approach, leading to evidence-based and
sustainable solutions;
• We recognize that the concern with the health and welfare of humankind underpins
the three international drug control conventions, which, together with other
relevant international instruments, are the cornerstone of the international drug
control system;
203
Decision of the United Nations Chief Executives Board for Coordination (CEB/2018/2), Second regular
session of 2018, Manhasset, New York, 7 and 8 November 2018, available at:
https://www.unsceb.org/CEBPublicFiles/CEB-2018-2-SoD.pdf
45
•
We acknowledge that the conventions allow for sufficient flexibility for countries to
design and implement national drug policies according to their priorities and needs,
consistent with the principle of common and shared responsibility and applicable
international law;
• We acknowledge that the international drug control conventions, international
human rights treaties and other relevant instruments, and the 2030 Agenda for
Sustainable Development are complementary and mutually reinforcing. National
drug control programmes, strategies and policies should be designed and
implemented by States in accordance with their human rights obligations.
Scope and purpose
• To guide approaches across the UN system, stepping up efforts to ensure that no
one is left behind;
• To inspire planning and implementation of UN activities, including joint inter-agency
activities;
• To speak with one voice and raise awareness of the multifaceted nature of the world
drug problem.
Directions for action
In addition to our ongoing efforts, we commit to harnessing synergies and strengthening
inter-agency cooperation, making best use of the expertise within the UN system, to further
enhance consistent sharing of information and lessons learned as well as the production of
more comprehensive data on the impact of drug policies, including with a view to supporting
the implementation of the 2030 Agenda for Sustainable Development.
We, therefore, commit to stepping up our joint efforts and supporting each other to, inter
alia:
• To support the development and implementation of policies that put people,
health and human rights at the centre, by providing a scientific evidence-based,
available, accessible and affordable recovery-oriented continuum of care based
upon prevention, treatment and support; and promote a rebalancing of drug
policies and interventions towards public health approaches;
• To promote the increased investment in measures aimed at minimizing the
adverse public health consequences of drug abuse, by some referred to as harm
reduction, which reduce new HIV infections, improve health outcomes and
deliver broader social benefits by reducing pressure on health-care and criminal
justice systems;
• To ensure the provision of drug prevention, treatment, rehabilitation and general
support services, including health care and social protection also in prison
46
settings, ensuring that they are equivalent to and that they provide continuity of
care with those in the community;
• To ensure the respect for the dignity and human rights for people who use drugs
in all aspects of drug and social policies, including equal access by people who
use drugs to public services including housing, health care and education;
• To call for Universal Health Coverage (UHC) for people with drug use disorders
and positioning of drug use disorders as other health conditions that should be
included in the overall UHC framework in national health systems;
• To enhance access to controlled medicines for legitimate medical and scientific
purposes including the relief of pain and treatment of drug dependence;
• To enhance international support for effective capacity-building in developing
countries to support the implementation of all the Sustainable Development
Goals, including through North-South, South-South and triangular cooperation;
• To support the identification of prevalent, persistent and harmful psychoactive
drugs including new psychoactive substances and their associated health risks,
using global and regional agencies’ early warning and alert systems;
• To provide guidance and technical assistance to strengthen cross-border law
enforcement and judicial cooperation;
• To promote sustainable livelihoods through adequately-sequenced, well-funded
and long-term development-oriented drug policies in rural and urban areas
affected by illicit drug activities, including cultivation, production and trafficking,
bearing in mind environmental protection and sustainability;
• To promote alternatives to conviction and punishment in appropriate cases,
including the decriminalization of drug possession for personal use, and promote
the principle of proportionality; address prison overcrowding and over-
incarceration by people accused of drug crimes; support implementation of
effective criminal justice responses that ensure legal guarantees and due process
safeguards pertaining to criminal justice proceedings and ensure timely access to
legal aid and the right to a fair trial; and support practical measures to prohibit
arbitrary arrest and detention and torture;
• To call for changes in laws, policies and practices that threaten the health and
human rights of people;
• To promote measures aimed at reducing stigma and elimination of discrimination
and achieving universal coverage of evidence-based prevention, treatment, and
rehabilitation;

47
•
To cooperate to ensure human rights-based drug control and address impunity
for serious human rights violations in the context of drug control efforts;
• To assist Member States in implementing non-discriminatory policies, including
with regard to ethnicity, race, sex, language, religion, or other status;
• To promote the active involvement and participation of civil society and local
communities, including people who use drugs, as well as women and youth;
• To provide Member States with a necessary evidence base to make informed
policy decisions and to better understand the risks and benefits of new
approaches to drug control, including those relating to cannabis;
• To compile, analyse and produce data reflecting UN system-wide practices and
lessons-learned in drug-related matters, and produce system-wide data and
analysis, including in light of the 2019 Ministerial segment of the CND and the
advancement of the implementation of the 2030 Agenda for Sustainable
Development.
Accountability and operationalization
We commit to supporting each other’s activities, within our mandates, and to delivering
balanced, comprehensive, integrated, evidence-based, human rights-based, development-
oriented, and sustainable support to Member States in implementing joint commitments,
including the operational recommendations contained in the outcome document of the
2016 United Nations Special Session on the World Drug Problem.
With a view to ensuring coherent efforts to realise the commitments under this US System
Common Position and, in particular, coordinated data collection to promote scientific,
evidence-based implementation of international commitments,
204
we establish a UN-system
Coordination Task Team, led by UNODC, of interested UN system entities, including those
with expertise in the collection of drug-related data, within the framework of the Secretary-
General’s Executive Committee.
204
Working in line with the principles governing international statistical activities (E/CN.3/2006/13,
annex), as endorsed by the Committee for the Coordination of Statistical Activities.
48
Annex II
Summary of key messages based on the knowledge produced and
acquired by the UN system on drug-related matters
Entities of the UN system have a common and shared responsibility to work together to pursue
a coordinated, balanced and comprehensive approach, leading to evidence-based and
sustainable solutions. As shown in this brief, there is a body of solid evidence that can guide
the action of the UN system and Member States to ensure that policies and programmes are
effective and in line with international standards. Based on this evidence and on the UN System
Common Position, the following key messages guide UN action to support Member States with
cost-effective and humane solutions.
Overall approach
• When it comes to addressing stigma and discrimination, not only do health service
providers need to be educated, but people who use drugs should be protected from
human rights abuses and discrimination by law.
• People and their health and human rights need to be put at the centre, by providing a
scientific evidence-based, available, accessible and affordable recovery-oriented
continuum of care based upon prevention, treatment and support.
• There is the need to assist Member States in implementing non-discriminatory policies,
including with regard to ethnicity, race, sex, language, religion or other status.
• It is key to promote the active involvement and participation of civil society and local
communities, including people who use drugs, as well as women and youth.
• Investing in data collection, analysis and research, at national, regional and global levels,
based on international standards and best practices is required to generate the
evidence needed to make informed policy decisions and to better understand the risks
and benefits of new approaches to drug control, including those relating to cannabis.
Health, including the availability of and access to controlled medicines
• A respect for the dignity and human rights for people who use drugs must be ensured
in all aspects of drug and social policies, including equal access by people who use drugs
to public services such as housing, health care and education.
• There is the need to achieve Universal Health Coverage (UHC) for people who use drugs
and to position drug dependence and other drug-related issues as health conditions
that should be included in the overall UHC framework in national health systems.
• Treatment services for drug use disorders should comply with human rights obligations
and recognize the inherent dignity of all individuals. This includes responding to the
49
right to receive the highest attainable standard of health and well-being and ensuring
non-discrimination. All interventions offered should meet the highest ethical
requirements, following the application of the Universal Declaration of Human Rights
on treating all patients and clients with respect and empathy.
• Measures aimed at reducing stigma, the elimination of discrimination and achieving
universal coverage of evidence-based prevention, treatment and rehabilitation should
be promoted.
• The provision of drug prevention, treatment, rehabilitation and general support
services is a necessity, including health care and social protection also in prison settings,
ensuring that they are equivalent to and that they provide continuity of care with those
in the community; there is the need to invest also in data collection and information
systems to monitor the drug situation in prison settings.
• Increased investment in measures aimed at minimizing the adverse public health
consequences of drug use, which reduce new HIV and viral hepatitis infections, provide
treatment and care for drug users with HIV, TB and viral hepatitis, improve other health
outcomes and social reintegration of people who use drugs, and deliver broader social
benefits, including by reducing pressure on health care and criminal justice systems.
These interventions work and are cost-effective, while also helping introduce people
who use drugs to health and social services.
• Controlled drugs should be accessible for legitimate medical and scientific purposes,
including the relief of pain and treatment of drug dependence.
Prevention of and responses to drug-related crime
• Guidance and technical assistance provided to Member States strengthens cross-
border law enforcement and judicial cooperation. Support regional and international
cooperation following the model of regional centres.
• Changes are required in laws, policies and practices that threaten the health and
human rights of people.
• Ensuring human rights-based drug control and addressing impunity for serious human
rights violations in the context of drug control efforts requires cooperation.

50
Countering illicit traffic in narcotic drugs and psychotropic substances
• There is a need to change the target for success among law enforcement agencies:
from quantities seized to the dismantling of drug trafficking organizations. This requires
a higher level of sophistication and the development of a critical mass of basic
knowledge among law enforcement and specialized units. Organized criminal groups
are changing their business model, so law enforcement requires training to understand
these new dynamics and to design effective actions. Best results come when there is
effective coordination among national institutions.
• Community policing and precision policing using detailed data and information at local
level need to be enhanced. Law enforcement organizations should be trained where
needed to fully respect human rights and understand gender perspectives.
Cooperation and joint training between law enforcement and public health
professionals produces the best outcomes. When law enforcement cooperates with
public health, lives are saved, crime is reduced and health is improved.
Proportionate and effective policies and responses (including evidence on alternatives to
incarceration and decriminalization/depenalization of drug use)
• Alternatives to conviction and punishment in appropriate cases are to be promoted, as
is the non-criminalization of drug use and drug possession for personal use, while
espousing public health and administrative measures that seek to prevent illicit drug
use, including the promotion of the principle of proportionality; address prison
overcrowding and over-incarceration by people accused of drug crimes; support
implementation of effective criminal justice responses that ensure legal guarantees
and due process safeguards pertaining to criminal justice proceedings and ensure
timely access to legal aid and the right to a fair trial; and support practical measures to
prohibit arbitrary arrest and detention and torture. Proportionality can be
implemented in the different steps of designing criminal justice responses: in law, in
applying the law, and in sentencing. The Secretary General calls on Member States that
continue to impose and implement death sentences, to declare and implement a
moratorium on executions with a view to abolishing the death penalty.
205
States that
have not yet abolished the death penalty may only impose it for the “most serious
crimes,” under strict adherence to fair trial safeguards and due process, and it should
never be mandatory.
206
• The Tokyo Rules, the Bangkok Rules, the Mandela Rules, and the UN Principles and
Guidelines on Access to Legal Aid in Criminal Justice Systems, are practical instruments
to develop human rights-based criminal justice responses to drug crime and need to be
fully implemented; taking a people-orientated approach in designing a criminal justice
response that focuses on the offender rather than the offence is important.
205
A/HRC/39/19, para. 48.
206
Ibid., para. 54, and Capital punishment and implementation of the safeguards guaranteeing protection of the
rights of those facing the death penalty, E/2015/49, para. 130.
51
Legal guarantees and safeguards pertaining to criminal justice proceedings and the justice sector
(including legal aid and the right to a fair trial)
• There is a lack of information on access to legal aid and a fair trial for drug offences.
Promoting a fair trial and avoiding discrimination remains essential for criminal justice
responses, but more investment is needed to collect data and to regularly monitor the
implementation of these principles.
Alternative development
• Sustainable livelihoods need to be promoted through adequately-sequenced, well-
funded and long-term development-oriented drug policies in rural and urban areas
affected by illicit drug activities, including cultivation, production and trafficking,
bearing in mind environmental protection and sustainability, and the need to monitor
and evaluate alternative programmes to ensure that they provide an effective solution.
• It is essential that employment creation strategies focus not only on the provision of
decent work but also target the structural transformation needed to tackle the supply
side of the world drug problem. As highlighted in the United Nations Guiding Principles
on Alternative Development, employment programs at both local and national levels
should be designed through community dialogue and participation and aim to achieve
inclusive economic growth that contributes to poverty eradication.
New psychoactive substances (NPS)
• The identification of prevalent, persistent and harmful psychoactive drugs, including
new psychoactive substances and their associated health risks, is best achieved using
early warning and alert systems; an important component is understanding and taking
into consideration the impact of regulating NPS on marginalized groups of people who
use drugs.
• Services are required to minimize the adverse public health consequences of drug use,
and drug treatment services targeted at people who use NPS are needed.
Non-medical use of pharmaceuticals
• A broad range of interventions are needed to address the non-medical use of
pharmaceuticals: control and awareness and the monitoring of prescription practices,
as well as the promotion of the UN guidelines on prescriptions.
• It is necessary to maximize both the protection of health and access to prescription
medicines, while avoiding misuse and dependency.
52
Annex III
Examples of joint programmes between UN entities on drug-related
matters
UNODC
–
WHO
Treatment
U
NODC
–
WHO
NPS
UNODC
–
UNAIDS
–
WHO
–
World Bank
Joint estimates on PWID, HIV, HCV
ICU
–
UNODC
–
WHO
–
INCB
Access to controlled medicines
Civil society
–
UNAIDS
–
WHO
–
UN Women
– UNDP
Global partnership to end all forms of
discrimination
Inter-Agency Technical Working Group on
Drug Epidemiology (WHO, UNODC, UNAIDS,
AU, EMCDDA, OAS, Pompidou Group)
Drug statistics
UNODC
–
WCO
Container Control Program
UNODC
–
INTERPOL
–
Transparency
International
CRIMJUST: strengthening criminal
investigation and criminal justice
cooperation along the cocaine routes in
Latin America, the Caribbean and West
Africa
UNODC – Interpol – WCO Airport Communication Project (AIRCOP)
UNESCO
–
UNODC
–
WHO
Effective education sector responses
UNODC
–
UNOWAS
–
Department of
Political and Peacebuilding Affairs (DPPA) –
Department of Peace Operations (DPO) –
INTERPOL
West African Coast Initiative (WACI)
